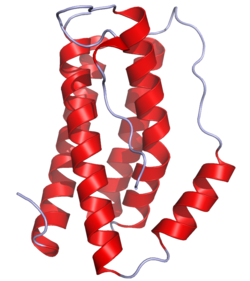
Interleukin 6 (IL-6) is an interleukin that acts as both a pro-inflammatory cytokine and an anti-inflammatory myokine. In humans, it is encoded by the IL6 gene.[5]
In addition, osteoblasts secrete IL-6 to stimulate osteoclast formation. Smooth muscle cells in the tunica media of many blood vessels also produce IL-6 as a pro-inflammatory cytokine. IL-6's role as an anti-inflammatory myokine is mediated through its inhibitory effects on TNF-alpha and IL-1 and its activation of IL-1ra and IL-10.
There is some early evidence that IL-6 can be used as an inflammatory marker for severe COVID-19 infection with poor prognosis, in the context of the wider coronavirus pandemic.[6]
Function
editImmune system
editIL-6 is secreted by macrophages in response to specific microbial molecules, referred to as pathogen-associated molecular patterns (PAMPs). These PAMPs bind to an important group of detection molecules of the innate immune system, called pattern recognition receptors (PRRs), including Toll-like receptors (TLRs). These are present on the cell surface and intracellular compartments and induce intracellular signaling cascades that give rise to inflammatory cytokine production. IL-6 is an important mediator of fever and of the acute phase response.
IL-6 is responsible for stimulating acute phase protein synthesis, as well as the production of neutrophils in the bone marrow. It supports the growth of B cells and is antagonistic to regulatory T cells.
Metabolic
editIt is capable of crossing the blood–brain barrier[7] and initiating synthesis of PGE2 in the hypothalamus, thereby changing the body's temperature setpoint. In muscle and fatty tissue, IL-6 stimulates energy mobilization that leads to increased body temperature. At 4 °C, both the oxygen consumption and core temperature were lower in IL-6-/- compared with wild-type mice, suggesting a lower cold-induced thermogenesis in IL-6-/- mice.[8]
In the absence of inflammation 10–35% of circulating IL-6 may come from adipose tissue.[9] IL-6 is produced by adipocytes and is thought to be a reason why obese individuals have higher endogenous levels of CRP.[10] IL-6 may exert a tonic suppression of body fat in mature mice, given that IL-6 gene knockout causes mature onset obesity.[11][12][13] Moreover, IL-6 can suppress body fat mass via effects at the level of the CNS.[11] The antiobesity effect of IL-6 in rodents is exerted at the level of the brain, presumably the hypothalamus and the hindbrain.[14][15][16] On the other hand, enhanced central IL-6 trans-signaling may improve energy and glucose homeostasis in obesity[17] Trans-signaling implicates that a soluble form of IL-6R (sIL-6R) comprising the extracellular portion of the receptor can bind IL-6 with a similar affinity as the membrane bound IL-6R. The complex of IL-6 and sIL-6R can bind to gp130 on cells, which do not express the IL-6R, and which are unresponsive to IL-6.[17]
Studies in experimental animals indicate that IL-6 in the CNS partly mediates the suppression of food intake and body weight exerted by glucagon-like peptide-1 (GLP-1) receptor stimulation.[18]
Outside the CNS, it seems that IL-6 stimulates the production of GLP-1 in the endocrine pancreas and the gut.[19] Amylin is another substance that can reduce body weight, and that may interact with IL-6. Amylin-induced IL-6 production in the ventromedial hypothalamus (VMH) is a possible mechanism by which amylin treatment could interact with VMH leptin signaling to increase its effect on weight loss.[20]
It is assumed that interleukin 6 in the liver activates the homologue of the human longevity gene mINDY expression via binding to its IL-6-receptor, which is associated with activation of the transcription factor STAT3 (which binds to the binding site in the mIndy promoter) and thereby rise of citrate uptake and hepatic lipogenesis.[21][22]
Central nervous system
editIntranasally administered IL-6 has been shown to improve sleep-associated consolidation of emotional memories.[23]
There are indications of interactions between GLP-1 and IL-6 in several parts of the brain. One example is the parabrachial nuclei of the pons, where GLP-1 increases IL-6 levels[24][25] and where IL-6 exerts a marked anti-obesity effect.[26]
Role as myokine
editIL-6 is also considered a myokine, a cytokine produced from muscle, which is elevated in response to muscle contraction.[27] It is significantly elevated with exercise, and precedes the appearance of other cytokines in the circulation. During exercise, it is thought to act in a hormone-like manner to mobilize extracellular substrates and/or augment substrate delivery.[28]
Like in humans, there seems to be an increase in IL-6 expression in working muscle and plasma IL-6 concentration during exercise in rodents.[29][30] Studies in mice with IL-6 gene knockout indicate that lack of IL-6 in mice affect exercise function.[9]
It has been shown that the reduction of abdominal obesity by exercise in human adults can be reversed by the IL-6 receptor blocking antibody tocilizumab. Together with the findings that IL-6 prevents obesity, stimulates lipolysis and is released from skeletal muscle during exercise, the tocilizumab finding indicates that IL-6 is required for exercise to reduce visceral adipose tissue mass.[31] Bone may be another organ affected by exercise induced IL-6, given that muscle-derived interleukin 6 has been reported to increase exercise capacity by signaling in osteoblasts.[32]
IL-6 has extensive anti-inflammatory functions in its role as a myokine. IL-6 was the first myokine that was found to be secreted into the blood stream in response to muscle contractions.[33] Aerobic exercise provokes a systemic cytokine response, including, for example, IL-6, IL-1 receptor antagonist (IL-1ra), and IL-10. IL-6 was serendipitously discovered as a myokine because of the observation that it increased in an exponential fashion proportional to the length of exercise and the amount of muscle mass engaged in the exercise. It has been consistently demonstrated that the plasma concentration of IL-6 increases during muscular exercise. This increase is followed by the appearance of IL-1ra and the anti-inflammatory cytokine IL-10. In general, the cytokine response to exercise and sepsis differs with regard to TNF-α. Thus, the cytokine response to exercise is not preceded by an increase in plasma-TNF-α. Following exercise, the basal plasma IL-6 concentration may increase up to 100-fold, but less dramatic increases are more frequent. The exercise-induced increase of plasma IL-6 occurs in an exponential manner and the peak IL-6 level is reached at the end of the exercise or shortly thereafter. It is the combination of mode, intensity, and duration of the exercise that determines the magnitude of the exercise-induced increase of plasma IL-6.[34]
IL-6 had previously been classified as a proinflammatory cytokine. Therefore, it was first thought that the exercise-induced IL-6 response was related to muscle damage.[35] However, it has become evident that eccentric exercise is not associated with a larger increase in plasma IL-6 than exercise involving concentric "nondamaging" muscle contractions. This finding clearly demonstrates that muscle damage is not required to provoke an increase in plasma IL-6 during exercise. As a matter of fact, eccentric exercise may result in a delayed peak and a much slower decrease of plasma IL-6 during recovery.[34]
Recent work has shown that both upstream and downstream signalling pathways for IL-6 differ markedly between myocytes and macrophages. It appears that unlike IL-6 signalling in macrophages, which is dependent upon activation of the NFκB signalling pathway, intramuscular IL-6 expression is regulated by a network of signalling cascades, including the Ca2+/NFAT and glycogen/p38 MAPK pathways. Thus, when IL-6 is signalling in monocytes or macrophages, it creates a pro-inflammatory response, whereas IL-6 activation and signalling in muscle is totally independent of a preceding TNF-response or NFκB activation, and is anti-inflammatory.[36]
IL-6, among an increasing number of other recently identified myokines, thus remains an important topic in myokine research. It appears in muscle tissue and in the circulation during exercise at levels up to one hundred times basal rates, as noted, and is seen as having a beneficial impact on health and bodily functioning when elevated in response to physical exercise.[37]
Receptor
editIL-6 signals through a cell-surface type I cytokine receptor complex consisting of the ligand-binding IL-6Rα chain (CD126), and the signal-transducing component gp130 (also called CD130). CD130 is the common signal transducer for several cytokines including leukemia inhibitory factor (LIF), ciliary neurotropic factor, oncostatin M, IL-11 and cardiotrophin-1, and is almost ubiquitously expressed in most tissues. In contrast, the expression of CD126 is restricted to certain tissues. As IL-6 interacts with its receptor, it triggers the gp130 and IL-6R proteins to form a complex, thus activating the receptor. These complexes bring together the intracellular regions of gp130 to initiate a signal transduction cascade through certain transcription factors, Janus kinases (JAKs) and Signal Transducers and Activators of Transcription (STATs).[38]
IL-6 is probably the best-studied of the cytokines that use gp130, also known as IL-6 signal transducer (IL6ST), in their signalling complexes. Other cytokines that signal through receptors containing gp130 are Interleukin 11 (IL-11), Interleukin 27 (IL-27), ciliary neurotrophic factor (CNTF), cardiotrophin-1 (CT-1), cardiotrophin-like cytokine (CLC), leukemia inhibitory factor (LIF), oncostatin M (OSM), Kaposi's sarcoma-associated herpesvirus interleukin 6-like protein (KSHV-IL6).[39] These cytokines are commonly referred to as the IL-6 like or gp130 utilising cytokines [40]
In addition to the membrane-bound receptor, a soluble form of IL-6R (sIL-6R) has been purified from human serum and urine. Many neuronal cells are unresponsive to stimulation by IL-6 alone, but differentiation and survival of neuronal cells can be mediated through the action of sIL-6R. The sIL-6R/IL-6 complex can stimulate neurites outgrowth and promote survival of neurons and, hence, may be important in nerve regeneration through remyelination.
Interactions
editInterleukin-6 has been shown to interact with interleukin-6 receptor,[41][42][43] glycoprotein 130,[44] and Galectin-3.[45]
There is considerable functional overlap and interaction between Substance P (SP), the natural ligand for the neurokinin type 1 receptor (NK1R, a mediator of immunomodulatory activity) and IL-6.
Role in disease
editIL-6 stimulates the inflammatory and auto-immune processes in many diseases such as multiple sclerosis,[46] neuromyelitis optica spectrum disorder (NMOSD),[46] diabetes,[47] atherosclerosis,[48] gastric cancer,[49] depression,[50] Alzheimer's disease,[51] systemic lupus erythematosus,[52] multiple myeloma,[53] prostate cancer,[54] Behçet's disease,[55] rheumatoid arthritis,[56] and intracerebral hemorrhage.[57]
Hence, there is an interest in developing anti-IL-6 agents as therapy against many of these diseases.[58][59] The first such is tocilizumab, which has been approved for rheumatoid arthritis,[60] Castleman's disease[61] and systemic juvenile idiopathic arthritis.[62] Others are in clinical trials.[63] It has been observed that genetic inactivation of ZCCHC 6 suppresses IL‐6 expression and reduces the severity of experimental osteoarthritis in Mice.[64] Some plant derived small molecule such as Butein have been reported to inhibit IL-6 expression in IL-1β stimulated human chondrocytes.[65]
Liver diseases
editSince IL-6 is a well-known pleiotropic molecule, it plays a dual role in the pathogenesis of liver diseases. While it is necessary for promoting liver regeneration,[66] IL-6 is also a highly recognized marker of systemic inflammation and its association with mortality in liver diseases has been reported by multiple studies.[67][68][69][70][71] In patients with severe alcohol-associated hepatitis, IL-6 showed the most robust elevation among inflammatory cytokines compared to healthy controls with a further increase in non-survivors. In these patients, IL-6 was a predictor of short-term (28- and 90-day) mortality.[71]
Rheumatoid arthritis
editThe first FDA approved anti-IL-6 treatment was for rheumatoid arthritis.
Cancer
editAnti-IL-6 therapy was initially developed for treatment of autoimmune diseases, but due to the role of IL-6 in chronic inflammation, IL-6 blockade was also evaluated for cancer treatment.[72][73][74] IL-6 was seen to have roles in tumor microenvironment regulation,[75][74] production of breast cancer stem cell-like cells,[76] metastasis through down-regulation of E-cadherin,[77] and alteration of DNA methylation in oral cancer.[78]
Advanced/metastatic cancer patients have higher levels of IL-6 in their blood.[79] One example of this is pancreatic cancer, with noted elevation of IL-6 present in patients correlating with poor survival rates.[80]
Diseases
editEnterovirus 71
editHigh IL-6 levels are associated with the development of encephalitis in children and immunodeficient mouse models infected with Enterovirus 71; this highly contagious virus normally causes a milder illness called Hand, foot, and mouth disease but can cause life-threatening encephalitis in some cases. EV71 patients with a certain gene polymorphism in IL-6 also appear to be more susceptible to developing encephalitis.
Epigenetic modifications
editIL-6 has been shown to lead to several neurological diseases through its impact on epigenetic modification within the brain.[81][82] IL-6 activates the Phosphoinositide 3-kinase (PI3K) pathway, and a downstream target of this pathway is the protein kinase B (PKB) (Hodge et al., 2007). IL-6 activated PKB can phosphorylate the nuclear localization signal on DNA methyltransferase-1 (DNMT1).[83] This phosphorylation causes movement of DNMT1 to the nucleus, where it can be transcribed.[83] DNMT1 recruits other DNMTs, including DNMT3A and DNMT3B, which, as a complex, recruit HDAC1.[82] This complex adds methyl groups to CpG islands on gene promoters, repressing the chromatin structure surrounding the DNA sequence and inhibiting transcriptional machinery from accessing the gene to induce transcription.[82] Increased IL-6, therefore, can hypermethylate DNA sequences and subsequently decrease gene expression through its effects on DNMT1 expression.[84]
Schizophrenia
editThe induction of epigenetic modification by IL-6 has been proposed as a mechanism in the pathology of schizophrenia through the hypermethylation and repression of the GAD67 promoter.[82] This hypermethylation may potentially lead to the decreased GAD67 levels seen in the brains of people with schizophrenia.[85] GAD67 may be involved in the pathology of schizophrenia through its effect on GABA levels and on neural oscillations.[86] Neural oscillations occur when inhibitory GABAergic neurons fire synchronously and cause inhibition of a multitude of target excitatory neurons at the same time, leading to a cycle of inhibition and disinhibition.[86] These neural oscillations are impaired in schizophrenia, and these alterations may be responsible for both positive and negative symptoms of schizophrenia.[87]
Aging
editIL-6 is commonly found in the senescence-associated secretory phenotype (SASP) factors secreted by senescent cells (a toxic cell-type that increases with aging).[88][89] Cancer (a disease that increases with age) invasiveness is promoted primarily though the actions of the SASP factors metalloproteinase, chemokine, IL-6, and interleukin 8 (IL-8).[90][88] IL-6 and IL-8 are the most conserved and robust features of SASP.[91]
Myelodysplastic Syndromes
IL-6 receptor was found upregulated in high-risk MDS patients. The inhibition of IL-6 signaling pathway can significantly ameliorate the clonogenicity of MDS hematopoietic stem and progenitor cells (HSPCs), but have undetectable effect on normal HSPCs.[74]
Depression and major depressive disorder
editThe epigenetic effects IL-6 have also been implicated in the pathology of depression. The effects of IL-6 on depression are mediated through the repression of brain-derived neurotrophic factor (BDNF) expression in the brain; DNMT1 hypermethylates the BDNF promoter and reduces BDNF levels.[92] Altered BDNF function has been implicated in depression,[93] which is likely due to epigenetic modification following IL-6 upregulation.[92] BDNF is a neurotrophic factor implicated in spine formation, density, and morphology on neurons.[94] Downregulation of BDNF, therefore, may cause decreased connectivity in the brain. Depression is marked by altered connectivity, in particular between the anterior cingulate cortex and several other limbic areas, such as the hippocampus.[95] The anterior cingulate cortex is responsible for detecting incongruences between expectation and perceived experience.[96] Altered connectivity of the anterior cingulate cortex in depression, therefore, may cause altered emotions following certain experiences, leading to depressive reactions.[96] This altered connectivity is mediated by IL-6 and its effect on epigenetic regulation of BDNF.[92]
Additional preclinical and clinical data, suggest that Substance P [SP] and IL-6 may act in concert to promote major depression. SP, a hybrid neurotransmitter-cytokine, is co-transmitted with BDNF through paleo-spinothalamic circuitry from the periphery with collaterals into key areas of the limbic system. However, both IL6 and SP mitigate expression of BDNF in brain regions associated with negative affect and memory. SP and IL6 both relax tight junctions of the blood brain barrier, such that effects seen in fMRI experiments with these molecules may be a bidirectional mix of neuronal, glial, capillary, synaptic, paracrine, or endocrine-like effects. At the cellular level, SP is noted to increase expression of interleukin-6 (IL-6) through PI-3K, p42/44 and p38 MAP kinase pathways. Data suggest that nuclear translocation of NF-κB regulates IL-6 overexpression in SP-stimulated cells.[97] This is of key interest as: 1) a meta-analysis indicates an association of major depressive disorder, C-reactive protein and IL6 plasma concentrations,[98] 2) NK1R antagonists [five molecules] studied by 3 independent groups in over 2000 patients from 1998 to 2013 validate the mechanism as dose-related, fully effective antidepressant, with a unique safety profile.[99][100] (see Summary of NK1RAs in Major Depression), 3) the preliminary observation that plasma concentrations of IL6 are elevated in depressed patients with cancer,[101] and 4) selective NK1RAs may eliminate endogenous SP stress-induced augmentation of IL-6 secretion pre-clinically.[102] These and many other reports suggest that a clinical study of a neutralizing IL-6 biological or drug based antagonist is likely warranted in patients with major depressive disorder, with or without co-morbid chronic inflammatory based illnesses; that the combination of NK1RAs and IL6 blockers may represent a new, potentially biomarkable approach to major depression, and possibly bipolar disorder.
The IL-6 antibody sirukumab underwent clinical trials for adjunctive treatment of major depressive disorder in 2015—2018,[103] but this research has been discontinued.[104]
Asthma
editObesity is a known risk factor in the development of severe asthma. Recent data suggests that the inflammation associated with obesity, potentially mediated by IL-6, plays a role in causing poor lung function and increased risk for developing asthma exacerbations.[105]
Protein superfamily
editInterleukin is the main member of the IL-6 superfamily (Pfam PF00489), which also includes G-CSF, IL23A, and CLCF1. A viral version of IL6 is found in Kaposi's sarcoma-associated herpesvirus.[106]
See also
edit- Ziltivekimab, a fully human monoclonal antibody against interleukin 6.
References
edit- ^ a b c GRCh38: Ensembl release 89: ENSG00000136244 – Ensembl, May 2017
- ^ a b c GRCm38: Ensembl release 89: ENSMUSG00000025746 – Ensembl, May 2017
- ^ "Human PubMed Reference:". National Center for Biotechnology Information, U.S. National Library of Medicine.
- ^ "Mouse PubMed Reference:". National Center for Biotechnology Information, U.S. National Library of Medicine.
- ^ Ferguson-Smith AC, Chen YF, Newman MS, May LT, Sehgal PB, Ruddle FH (April 1988). "Regional localization of the interferon-beta 2/B-cell stimulatory factor 2/hepatocyte stimulating factor gene to human chromosome 7p15-p21". Genomics. 2 (3): 203–208. doi:10.1016/0888-7543(88)90003-1. PMID 3294161.
- ^ "Raised troponin and interleukin-6 levels are associated with a poor prognosis in COVID-19". Cardiac Rhythm News. 2 April 2020.
- ^ Banks WA, Kastin AJ, Gutierrez EG (September 1994). "Penetration of interleukin-6 across the murine blood–brain barrier". Neuroscience Letters. 179 (1–2): 53–56. doi:10.1016/0304-3940(94)90933-4. PMID 7845624. S2CID 22712577.
- ^ Wernstedt I, Edgley A, Berndtsson A, Fäldt J, Bergström G, Wallenius V, et al. (September 2006). "Reduced stress- and cold-induced increase in energy expenditure in interleukin-6-deficient mice". American Journal of Physiology. Regulatory, Integrative and Comparative Physiology. 291 (3): R551–R557. doi:10.1152/ajpregu.00514.2005. PMID 16455769.
- ^ a b Fäldt J, Wernstedt I, Fitzgerald SM, Wallenius K, Bergström G, Jansson JO (June 2004). "Reduced exercise endurance in interleukin-6-deficient mice". Endocrinology. 145 (6): 2680–2686. doi:10.1210/en.2003-1319. PMID 14988384.
- ^ Bastard JP, Jardel C, Delattre J, Hainque B, Bruckert E, Oberlin F (April 1999). "Evidence for a link between adipose tissue interleukin-6 content and serum C-reactive protein concentrations in obese subjects". Circulation. 99 (16): 2221–2222. doi:10.1161/circ.99.16.2219/c. PMID 10217702.
- ^ a b Wallenius V, Wallenius K, Ahrén B, Rudling M, Carlsten H, Dickson SL, et al. (January 2002). "Interleukin-6-deficient mice develop mature-onset obesity". Nature Medicine. 8 (1): 75–79. doi:10.1038/nm0102-75. PMID 11786910. S2CID 7111589.
- ^ Matthews VB, Allen TL, Risis S, Chan MH, Henstridge DC, Watson N, et al. (November 2010). "Interleukin-6-deficient mice develop hepatic inflammation and systemic insulin resistance". Diabetologia. 53 (11): 2431–2441. doi:10.1007/s00125-010-1865-y. PMID 20697689. S2CID 12970519.
- ^ Di Gregorio GB, Hensley L, Lu T, Ranganathan G, Kern PA (July 2004). "Lipid and carbohydrate metabolism in mice with a targeted mutation in the IL-6 gene: absence of development of age-related obesity". American Journal of Physiology. Endocrinology and Metabolism. 287 (1): E182–E187. doi:10.1152/ajpendo.00189.2003. PMID 15191885.
- ^ Wallenius K, Wallenius V, Sunter D, Dickson SL, Jansson JO (April 2002). "Intracerebroventricular interleukin-6 treatment decreases body fat in rats". Biochemical and Biophysical Research Communications. 293 (1): 560–565. doi:10.1016/S0006-291X(02)00230-9. PMID 12054638.
- ^ Sadagurski M, Norquay L, Farhang J, D'Aquino K, Copps K, White MF (March 2010). "Human IL6 enhances leptin action in mice". Diabetologia. 53 (3): 525–535. doi:10.1007/s00125-009-1580-8. PMC 2815798. PMID 19902173.
- ^ Campbell IL, Erta M, Lim SL, Frausto R, May U, Rose-John S, et al. (February 2014). "Trans-signaling is a dominant mechanism for the pathogenic actions of interleukin-6 in the brain". The Journal of Neuroscience. 34 (7): 2503–2513. doi:10.1523/JNEUROSCI.2830-13.2014. PMC 6802757. PMID 24523541.
- ^ a b Rose-John S (2012). "IL-6 trans-signaling via the soluble IL-6 receptor: importance for the pro-inflammatory activities of IL-6". International Journal of Biological Sciences. 8 (9): 1237–1247. doi:10.7150/ijbs.4989. PMC 3491447. PMID 23136552.
- ^ Shirazi R, Palsdottir V, Collander J, Anesten F, Vogel H, Langlet F, et al. (October 2013). "Glucagon-like peptide 1 receptor induced suppression of food intake, and body weight is mediated by central IL-1 and IL-6". Proceedings of the National Academy of Sciences of the United States of America. 110 (40): 16199–16204. Bibcode:2013PNAS..11016199S. doi:10.1073/pnas.1306799110. PMC 3791711. PMID 24048027.
- ^ Ellingsgaard H, Hauselmann I, Schuler B, Habib AM, Baggio LL, Meier DT, et al. (October 2011). "Interleukin-6 enhances insulin secretion by increasing glucagon-like peptide-1 secretion from L cells and alpha cells". Nature Medicine. 17 (11): 1481–1489. doi:10.1038/nm.2513. PMC 4286294. PMID 22037645.
- ^ Le Foll C, Johnson MD, Dunn-Meynell AA, Boyle CN, Lutz TA, Levin BE (May 2015). "Amylin-induced central IL-6 production enhances ventromedial hypothalamic leptin signaling". Diabetes. 64 (5): 1621–1631. doi:10.2337/db14-0645. PMC 4407855. PMID 25409701.
- ^ von Loeffelholz C, Lieske S, Neuschäfer-Rube F, Willmes DM, Raschzok N, Sauer IM, et al. (August 2017). "The human longevity gene homolog INDY and interleukin-6 interact in hepatic lipid metabolism". Hepatology. 66 (2): 616–630. doi:10.1002/hep.29089. PMC 5519435. PMID 28133767.
- ^ Rogina B (2017). "INDY-A New Link to Metabolic Regulation in Animals and Humans". Frontiers in Genetics. 8: 66. doi:10.3389/fgene.2017.00066. PMC 5442177. PMID 28596784. This article incorporates text from this source, which is available under the CC BY 4.0 license.
- ^ Benedict C, Scheller J, Rose-John S, Born J, Marshall L (October 2009). "Enhancing influence of intranasal interleukin-6 on slow-wave activity and memory consolidation during sleep". FASEB Journal. 23 (10): 3629–3636. doi:10.1096/fj.08-122853. PMID 19546306. S2CID 38515607.
- ^ Richard JE, Farkas I, Anesten F, Anderberg RH, Dickson SL, Gribble FM, et al. (November 2014). "GLP-1 receptor stimulation of the lateral parabrachial nucleus reduces food intake: neuroanatomical, electrophysiological, and behavioral evidence". Endocrinology. 155 (11): 4356–4367. doi:10.1210/en.2014-1248. PMC 4256827. PMID 25116706.
- ^ Anesten F, Mishra D, Dalmau Gasull A, Engström-Ruud L, Bellman J, Palsdottir V, et al. (2019). "Glucagon-Like Peptide-1-, but not Growth and Differentiation Factor 15-, Receptor Activation Increases the Number of Interleukin-6-Expressing Cells in the External Lateral Parabrachial Nucleus". Neuroendocrinology. 109 (4): 310–321. doi:10.1159/000499693. PMID 30889580. S2CID 208014066.
- ^ Mishra D, Richard JE, Maric I, Porteiro B, Häring M, Kooijman S, et al. (March 2019). "Parabrachial Interleukin-6 Reduces Body Weight and Food Intake and Increases Thermogenesis to Regulate Energy Metabolism". Cell Reports. 26 (11): 3011–3026.e5. doi:10.1016/j.celrep.2019.02.044. PMC 6418345. PMID 30865890.
- ^ Febbraio MA, Pedersen BK (July 2005). "Contraction-induced myokine production and release: is skeletal muscle an endocrine organ?". Exercise and Sport Sciences Reviews. 33 (3): 114–119. doi:10.1097/00003677-200507000-00003. PMID 16006818. S2CID 26503323.
- ^ Petersen AM, Pedersen BK (April 2005). "The anti-inflammatory effect of exercise". Journal of Applied Physiology. 98 (4): 1154–1162. doi:10.1152/japplphysiol.00164.2004. PMID 15772055. S2CID 4776835.
- ^ Colbert LH, Davis JM, Essig DA, Ghaffar A, Mayer EP (May 2001). "Tissue expression and plasma concentrations of TNFalpha, IL-1beta, and IL-6 following treadmill exercise in mice". International Journal of Sports Medicine. 22 (4): 261–267. doi:10.1055/s-2001-13818. PMID 11414667. S2CID 260192304.
- ^ Jonsdottir IH, Schjerling P, Ostrowski K, Asp S, Richter EA, Pedersen BK (October 2000). "Muscle contractions induce interleukin-6 mRNA production in rat skeletal muscles". The Journal of Physiology. 528 Pt 1 (Pt 1): 157–163. doi:10.1111/j.1469-7793.2000.00157.x. PMC 2270126. PMID 11018114.
- ^ Wedell-Neergaard AS, Lang Lehrskov L, Christensen RH, Legaard GE, Dorph E, Larsen MK, et al. (April 2019). "Exercise-Induced Changes in Visceral Adipose Tissue Mass Are Regulated by IL-6 Signaling: A Randomized Controlled Trial". Cell Metabolism. 29 (4): 844–855.e3. doi:10.1016/j.cmet.2018.12.007. PMID 30595477.
- ^ Chowdhury S, Schulz L, Palmisano B, Singh P, Berger JM, Yadav VK, et al. (June 2020). "Muscle-derived interleukin 6 increases exercise capacity by signaling in osteoblasts". The Journal of Clinical Investigation. 130 (6): 2888–2902. doi:10.1172/JCI133572. PMC 7260002. PMID 32078586.
- ^ Pedersen BK, Febbraio MA (October 2008). "Muscle as an endocrine organ: focus on muscle-derived interleukin-6". Physiological Reviews. 88 (4): 1379–1406. doi:10.1152/physrev.90100.2007. PMID 18923185. S2CID 12601630.
- ^ a b Pedersen BK (July 2013). "Muscle as a secretory organ". Comprehensive Physiology. Vol. 3. pp. 1337–62. doi:10.1002/cphy.c120033. ISBN 9780470650714. PMID 23897689.
- ^ Bruunsgaard H, Galbo H, Halkjaer-Kristensen J, Johansen TL, MacLean DA, Pedersen BK (March 1997). "Exercise-induced increase in serum interleukin-6 in humans is related to muscle damage". The Journal of Physiology. 499 (Pt 3) (3): 833–841. doi:10.1113/jphysiol.1997.sp021972. PMC 1159298. PMID 9130176.
- ^ Brandt C, Pedersen BK (2010). "The role of exercise-induced myokines in muscle homeostasis and the defense against chronic diseases". Journal of Biomedicine & Biotechnology. 2010: 520258. doi:10.1155/2010/520258. PMC 2836182. PMID 20224659.
- ^ Muñoz-Cánoves P, Scheele C, Pedersen BK, Serrano AL (September 2013). "Interleukin-6 myokine signaling in skeletal muscle: a double-edged sword?". The FEBS Journal. 280 (17): 4131–4148. doi:10.1111/febs.12338. PMC 4163639. PMID 23663276.
- ^ Heinrich PC, Behrmann I, Müller-Newen G, Schaper F, Graeve L (September 1998). "Interleukin-6-type cytokine signalling through the gp130/Jak/STAT pathway". The Biochemical Journal. 334 (Pt 2) (Pt 2): 297–314. doi:10.1042/bj3340297. PMC 1219691. PMID 9716487.
- ^ Kishimoto T, Akira S, Narazaki M, Taga T (August 1995). "Interleukin-6 family of cytokines and gp130". Blood. 86 (4): 1243–1254. doi:10.1182/blood.V86.4.1243.bloodjournal8641243. PMID 7632928.
- ^ Heinrich PC, Behrmann I, Haan S, Hermanns HM, Müller-Newen G, Schaper F (August 2003). "Principles of interleukin (IL)-6-type cytokine signalling and its regulation". The Biochemical Journal. 374 (Pt 1): 1–20. doi:10.1042/BJ20030407. PMC 1223585. PMID 12773095.
- ^ Schwantner A, Dingley AJ, Ozbek S, Rose-John S, Grötzinger J (January 2004). "Direct determination of the interleukin-6 binding epitope of the interleukin-6 receptor by NMR spectroscopy". The Journal of Biological Chemistry. 279 (1): 571–576. doi:10.1074/jbc.M311019200. PMID 14557255.
- ^ Schuster B, Kovaleva M, Sun Y, Regenhard P, Matthews V, Grötzinger J, et al. (March 2003). "Signaling of human ciliary neurotrophic factor (CNTF) revisited. The interleukin-6 receptor can serve as an alpha-receptor for CTNF". The Journal of Biological Chemistry. 278 (11): 9528–9535. doi:10.1074/jbc.M210044200. PMID 12643274.
- ^ Taga T, Hibi M, Hirata Y, Yamasaki K, Yasukawa K, Matsuda T, et al. (August 1989). "Interleukin-6 triggers the association of its receptor with a possible signal transducer, gp130". Cell. 58 (3): 573–581. doi:10.1016/0092-8674(89)90438-8. PMID 2788034. S2CID 41245022.
- ^ Kallen KJ, zum Büschenfelde KH, Rose-John S (March 1997). "The therapeutic potential of interleukin-6 hyperagonists and antagonists". Expert Opinion on Investigational Drugs. 6 (3): 237–266. doi:10.1517/13543784.6.3.237. PMID 15989626.
- ^ Gordon-Alonso M, Bruger AM, van der Bruggen P (August 2018). "Extracellular galectins as controllers of cytokines in hematological cancer". Blood. 132 (5): 484–491. doi:10.1182/blood-2018-04-846014. PMC 6073326. PMID 29875102.
- ^ a b Kong BS, Kim Y, Kim GY, Hyun JW, Kim SH, Jeong A, et al. (September 2017). "Increased frequency of IL-6-producing non-classical monocytes in neuromyelitis optica spectrum disorder". Journal of Neuroinflammation. 14 (1): 191. doi:10.1186/s12974-017-0961-z. PMC 5613387. PMID 28946890.
- ^ Kristiansen OP, Mandrup-Poulsen T (December 2005). "Interleukin-6 and diabetes: the good, the bad, or the indifferent?". Diabetes. 54 (Suppl 2): S114–S124. doi:10.2337/diabetes.54.suppl_2.S114. PMID 16306329.
- ^ Dubiński A, Zdrojewicz Z (April 2007). "[The role of interleukin-6 in development and progression of atherosclerosis]". Polski Merkuriusz Lekarski (in Polish). 22 (130): 291–294. PMID 17684929.
- ^ Yu B, de Vos D, Guo X, Peng S, Xie W, Peppelenbosch MP, et al. (April 2024). "IL-6 facilitates cross-talk between epithelial cells and tumor- associated macrophages in Helicobacter pylori-linked gastric carcinogenesis". Neoplasia. 50: 100981. doi:10.1016/j.neo.2024.100981. PMC 10912637. PMID 38422751.
- ^ Dowlati Y, Herrmann N, Swardfager W, Liu H, Sham L, Reim EK, et al. (March 2010). "A meta-analysis of cytokines in major depression". Biological Psychiatry. 67 (5): 446–457. doi:10.1016/j.biopsych.2009.09.033. PMID 20015486. S2CID 230209.
- ^ Swardfager W, Lanctôt K, Rothenburg L, Wong A, Cappell J, Herrmann N (November 2010). "A meta-analysis of cytokines in Alzheimer's disease". Biological Psychiatry. 68 (10): 930–941. doi:10.1016/j.biopsych.2010.06.012. PMID 20692646. S2CID 6544784.
- ^ Tackey E, Lipsky PE, Illei GG (2004). "Rationale for interleukin-6 blockade in systemic lupus erythematosus". Lupus. 13 (5): 339–343. doi:10.1191/0961203304lu1023oa. PMC 2014821. PMID 15230289.
- ^ Gadó K, Domján G, Hegyesi H, Falus A (2000). "Role of INTERLEUKIN-6 in the pathogenesis of multiple myeloma". Cell Biology International. 24 (4): 195–209. doi:10.1006/cbir.2000.0497. PMID 10816321. S2CID 44820455.
- ^ Smith PC, Hobisch A, Lin DL, Culig Z, Keller ET (March 2001). "Interleukin-6 and prostate cancer progression". Cytokine & Growth Factor Reviews. 12 (1): 33–40. doi:10.1016/S1359-6101(00)00021-6. PMID 11312117.
- ^ Hirohata S, Kikuchi H (Dec 2012). "Changes in biomarkers focused on differences in disease course or treatment in patients with neuro-Behçet's disease". Internal Medicine. 51 (24): 3359–3365. doi:10.2169/internalmedicine.51.8583. PMID 23257520.
- ^ Nishimoto N (May 2006). "Interleukin-6 in rheumatoid arthritis". Current Opinion in Rheumatology. 18 (3): 277–281. doi:10.1097/01.bor.0000218949.19860.d1. PMID 16582692. S2CID 20188179.
- ^ Zhu H, Wang Z, Yu J, Yang X, He F, Liu Z, et al. (July 2019). "Role and mechanisms of cytokines in the secondary brain injury after intracerebral hemorrhage". Progress in Neurobiology. 178: 101610. doi:10.1016/j.pneurobio.2019.03.003. PMID 30923023. S2CID 85495400.
- ^ Barton BE (August 2005). "Interleukin-6 and new strategies for the treatment of cancer, hyperproliferative diseases and paraneoplastic syndromes". Expert Opinion on Therapeutic Targets. 9 (4): 737–752. doi:10.1517/14728222.9.4.737. PMID 16083340. S2CID 45421426.
- ^ Smolen JS, Maini RN (2006). "Interleukin-6: a new therapeutic target". Arthritis Research & Therapy. 8 (Suppl 2): S5. doi:10.1186/ar1969. PMC 3226077. PMID 16899109.
- ^ Emery P, Keystone E, Tony HP, Cantagrel A, van Vollenhoven R, Sanchez A, et al. (November 2008). "IL-6 receptor inhibition with tocilizumab improves treatment outcomes in patients with rheumatoid arthritis refractory to anti-tumour necrosis factor biologicals: results from a 24-week multicentre randomised placebo-controlled trial". Annals of the Rheumatic Diseases. 67 (11): 1516–1523. doi:10.1136/ard.2008.092932. PMC 3811149. PMID 18625622.
- ^ Nishimoto N, Kanakura Y, Aozasa K, Johkoh T, Nakamura M, Nakano S, et al. (October 2005). "Humanized anti-interleukin-6 receptor antibody treatment of multicentric Castleman disease". Blood. 106 (8): 2627–2632. doi:10.1182/blood-2004-12-4602. PMID 15998837.
- ^ Yokota S, Imagawa T, Mori M, Miyamae T, Aihara Y, Takei S, et al. (March 2008). "Efficacy and safety of tocilizumab in patients with systemic-onset juvenile idiopathic arthritis: a randomised, double-blind, placebo-controlled, withdrawal phase III trial". Lancet. 371 (9617): 998–1006. doi:10.1016/S0140-6736(08)60454-7. PMID 18358927. S2CID 21554759.
- ^ First IL-6–blocking drug nears approval for rare blood disorder, Nature Medicine, October 7, 2013
- ^ Ansari MY, Khan NM, Ahmad N, Green J, Novak K, Haqqi TM (April 2019). "Genetic Inactivation of ZCCHC6 Suppresses Interleukin-6 Expression and Reduces the Severity of Experimental Osteoarthritis in Mice". Arthritis & Rheumatology. 71 (4): 583–593. doi:10.1002/art.40751. ISSN 2326-5205. PMC 6438766. PMID 30302948.
- ^ Ansari MY, Ahmad N, Haqqi TM (2018). "Butein Activates Autophagy Through AMPK/TSC2/ULK1/mTOR Pathway to Inhibit IL-6 Expression in IL-1β Stimulated Human Chondrocytes". Cellular Physiology and Biochemistry: International Journal of Experimental Cellular Physiology, Biochemistry, and Pharmacology. 49 (3): 932–946. doi:10.1159/000493225. ISSN 1421-9778. PMID 30184535. S2CID 52166938.
- ^ Gao B, Ahmad MF, Nagy LE, Tsukamoto H (February 2019). "Inflammatory pathways in alcoholic steatohepatitis". Journal of Hepatology. 70 (2): 249–259. doi:10.1016/j.jhep.2018.10.023. PMC 6361545. PMID 30658726.
- ^ Remmler J, Schneider C, Treuner-Kaueroff T, Bartels M, Seehofer D, Scholz M, et al. (May 2018). "Increased Level of Interleukin 6 Associates With Increased 90-Day and 1-Year Mortality in Patients With End-Stage Liver Disease". Clinical Gastroenterology and Hepatology. 16 (5): 730–737. doi:10.1016/j.cgh.2017.09.017. PMID 28919544. S2CID 4408167.
- ^ Zhou C, Zhang N, He TT, Wang Y, Wang LF, Sun YQ, et al. (August 2020). "High levels of serum interleukin-6 increase mortality of hepatitis B virus-associated acute-on-chronic liver failure". World Journal of Gastroenterology. 26 (30): 4479–4488. doi:10.3748/wjg.v26.i30.4479. PMC 7438191. PMID 32874059.
- ^ Sheron N, Bird G, Goka J, Alexander G, Williams R (June 1991). "Elevated plasma interleukin-6 and increased severity and mortality in alcoholic hepatitis". Clinical and Experimental Immunology. 84 (3): 449–453. PMC 1535433. PMID 2044224.
- ^ Arroyo V, Angeli P, Moreau R, Jalan R, Clària J, Trebicka J, et al. (March 2021). "The systemic inflammation hypothesis: Towards a new paradigm of acute decompensation and multiorgan failure in cirrhosis". Journal of Hepatology. 74 (3): 670–685. doi:10.1016/j.jhep.2020.11.048. hdl:2445/175350. PMID 33301825.
- ^ a b Tornai D, Mitchell M, McClain CJ, Dasarathy S, McCullough A, Radaeva S, et al. (December 2023). "A novel score of IL-13 and age predicts 90-day mortality in severe alcohol-associated hepatitis: A multicenter plasma biomarker analysis". Hepatology Communications. 7 (12). doi:10.1097/HC9.0000000000000296. PMC 10666984. PMID 37994498.
- ^ Korneev KV, Atretkhany KN, Drutskaya MS, Grivennikov SI, Kuprash DV, Nedospasov SA (January 2017). "TLR-signaling and proinflammatory cytokines as drivers of tumorigenesis". Cytokine. 89: 127–135. doi:10.1016/j.cyto.2016.01.021. PMID 26854213.
- ^ Anestakis D, Petanidis S, Kalyvas S, Nday CM, Tsave O, Kioseoglou E, et al. (January 2015). "Mechanisms and applications of interleukins in cancer immunotherapy". International Journal of Molecular Sciences. 16 (1): 1691–1710. doi:10.3390/ijms16011691. PMC 4307328. PMID 25590298.
- ^ a b c Mei Y, Ren K, Liu Y, Ma A, Xia Z, Han X, et al. (September 2022). "Bone marrow-confined IL-6 signaling mediates the progression of myelodysplastic syndromes to acute myeloid leukemia". The Journal of Clinical Investigation. 132 (17): e152673. doi:10.1172/JCI152673. PMC 9435651. PMID 35900794.
- ^ Li J, Mo HY, Xiong G, Zhang L, He J, Huang ZF, et al. (October 2012). "Tumor microenvironment macrophage inhibitory factor directs the accumulation of interleukin-17-producing tumor-infiltrating lymphocytes and predicts favorable survival in nasopharyngeal carcinoma patients". The Journal of Biological Chemistry. 287 (42): 35484–35495. doi:10.1074/jbc.M112.367532. PMC 3471767. PMID 22893706.
- ^ Xie G, Yao Q, Liu Y, Du S, Liu A, Guo Z, et al. (April 2012). "IL-6-induced epithelial-mesenchymal transition promotes the generation of breast cancer stem-like cells analogous to mammosphere cultures". International Journal of Oncology. 40 (4): 1171–1179. doi:10.3892/ijo.2011.1275. PMC 3584811. PMID 22134360.
- ^ Miao JW, Liu LJ, Huang J (July 2014). "Interleukin-6-induced epithelial-mesenchymal transition through signal transducer and activator of transcription 3 in human cervical carcinoma". International Journal of Oncology. 45 (1): 165–176. doi:10.3892/ijo.2014.2422. PMID 24806843.
- ^ Gasche JA, Hoffmann J, Boland CR, Goel A (September 2011). "Interleukin-6 promotes tumorigenesis by altering DNA methylation in oral cancer cells". International Journal of Cancer. 129 (5): 1053–1063. doi:10.1002/ijc.25764. PMC 3110561. PMID 21710491.
- ^ "Cancer Patients Typically Have Increased Interleukin-6 Levels". American Society of Clinical Oncology 2006 Annual Meeting, Abstracts 8632 and 8633. Medscape.com. 2006-06-26.
- ^ Bellone G, Smirne C, Mauri FA, Tonel E, Carbone A, Buffolino A, et al. (June 2006). "Cytokine expression profile in human pancreatic carcinoma cells and in surgical specimens: implications for survival". Cancer Immunology, Immunotherapy. 55 (6): 684–698. doi:10.1007/s00262-005-0047-0. PMC 11031060. PMID 16094523. S2CID 11019678.
- ^ Smith SE, Li J, Garbett K, Mirnics K, Patterson PH (October 2007). "Maternal immune activation alters fetal brain development through interleukin-6". The Journal of Neuroscience. 27 (40): 10695–10702. doi:10.1523/JNEUROSCI.2178-07.2007. PMC 2387067. PMID 17913903.
- ^ a b c d Kundakovic M, Chen Y, Guidotti A, Grayson DR (February 2009). "The reelin and GAD67 promoters are activated by epigenetic drugs that facilitate the disruption of local repressor complexes". Molecular Pharmacology. 75 (2): 342–354. doi:10.1124/mol.108.051763. PMC 2684898. PMID 19029285.
- ^ a b Hodge DR, Cho E, Copeland TD, Guszczynski T, Yang E, Seth AK, et al. (2007). "IL-6 enhances the nuclear translocation of DNA cytosine-5-methyltransferase 1 (DNMT1) via phosphorylation of the nuclear localization sequence by the AKT kinase". Cancer Genomics & Proteomics. 4 (6): 387–398. PMID 18204201.
- ^ Foran E, Garrity-Park MM, Mureau C, Newell J, Smyrk TC, Limburg PJ, et al. (April 2010). "Upregulation of DNA methyltransferase-mediated gene silencing, anchorage-independent growth, and migration of colon cancer cells by interleukin-6". Molecular Cancer Research. 8 (4): 471–481. doi:10.1158/1541-7786.MCR-09-0496. PMID 20354000.
- ^ Guidotti A, Auta J, Davis JM, Di-Giorgi-Gerevini V, Dwivedi Y, Grayson DR, et al. (November 2000). "Decrease in reelin and glutamic acid decarboxylase67 (GAD67) expression in schizophrenia and bipolar disorder: a postmortem brain study". Archives of General Psychiatry. 57 (11): 1061–1069. doi:10.1001/archpsyc.57.11.1061. PMID 11074872.
- ^ a b Gandal MJ, Sisti J, Klook K, Ortinski PI, Leitman V, Liang Y, et al. (July 2012). "GABAB-mediated rescue of altered excitatory-inhibitory balance, gamma synchrony and behavioral deficits following constitutive NMDAR-hypofunction". Translational Psychiatry. 2 (7): e142. doi:10.1038/tp.2012.69. PMC 3410621. PMID 22806213.
- ^ Uhlhaas PJ, Singer W (February 2010). "Abnormal neural oscillations and synchrony in schizophrenia". Nature Reviews. Neuroscience. 11 (2): 100–113. doi:10.1038/nrn2774. PMID 20087360. S2CID 205505539.
- ^ a b Coppé JP, Patil CK, Rodier F, Sun Y, Muñoz DP, Goldstein J, et al. (December 2008). "Senescence-associated secretory phenotypes reveal cell-nonautonomous functions of oncogenic RAS and the p53 tumor suppressor". PLOS Biology. 6 (12): 2853–2868. doi:10.1371/journal.pbio.0060301. PMC 2592359. PMID 19053174.
- ^ Childs BG, Gluscevic M, Baker DJ, Laberge RM, Marquess D, Dananberg J, et al. (October 2017). "Senescent cells: an emerging target for diseases of ageing". Nature Reviews. Drug Discovery. 16 (10): 718–735. doi:10.1038/nrd.2017.116. PMC 5942225. PMID 28729727.
- ^ Kim YH, Park TJ (January 2019). "Cellular senescence in cancer". BMB Reports. 52 (1): 42–46. doi:10.5483/BMBRep.2019.52.1.295. PMC 6386235. PMID 30526772.
- ^ Partridge L, Fuentealba M, Kennedy BK (August 2020). "The quest to slow ageing through drug discovery". Nature Reviews. Drug Discovery. 19 (8): 513–532. doi:10.1038/s41573-020-0067-7. PMID 32467649. S2CID 218912510.
- ^ a b c Sharma RP, Tun N, Grayson DR (2008). "Depolarization induces downregulation of DNMT1 and DNMT3a in primary cortical cultures". Epigenetics. 3 (2): 74–80. doi:10.4161/epi.3.2.6103. PMID 18536530.
- ^ Hwang JP, Tsai SJ, Hong CJ, Yang CH, Lirng JF, Yang YM (December 2006). "The Val66Met polymorphism of the brain-derived neurotrophic-factor gene is associated with geriatric depression". Neurobiology of Aging. 27 (12): 1834–1837. doi:10.1016/j.neurobiolaging.2005.10.013. PMID 16343697. S2CID 23626890.
- ^ Ethell IM, Pasquale EB (February 2005). "Molecular mechanisms of dendritic spine development and remodeling". Progress in Neurobiology. 75 (3): 161–205. doi:10.1016/j.pneurobio.2005.02.003. PMID 15882774. S2CID 24889257.
- ^ Greicius MD, Flores BH, Menon V, Glover GH, Solvason HB, Kenna H, et al. (September 2007). "Resting-state functional connectivity in major depression: abnormally increased contributions from subgenual cingulate cortex and thalamus". Biological Psychiatry. 62 (5): 429–437. doi:10.1016/j.biopsych.2006.09.020. PMC 2001244. PMID 17210143.
- ^ a b Somerville LH, Heatherton TF, Kelley WM (August 2006). "Anterior cingulate cortex responds differentially to expectancy violation and social rejection". Nature Neuroscience. 9 (8): 1007–1008. doi:10.1038/nn1728. PMID 16819523. S2CID 35224855.
- ^ Azzolina A, Bongiovanni A, Lampiasi N (December 2003). "Substance P induces TNF-alpha and IL-6 production through NF kappa B in peritoneal mast cells". Biochimica et Biophysica Acta (BBA) - Molecular Cell Research. 1643 (1–3): 75–83. doi:10.1016/j.bbamcr.2003.09.003. PMID 14654230.
- ^ Haapakoski R, Mathieu J, Ebmeier KP, Alenius H, Kivimäki M (October 2015). "Cumulative meta-analysis of interleukins 6 and 1β, tumour necrosis factor α and C-reactive protein in patients with major depressive disorder". Brain, Behavior, and Immunity. 49: 206–215. doi:10.1016/j.bbi.2015.06.001. PMC 4566946. PMID 26065825.
- ^ Ratti E, Bettica P, Alexander R, Archer G, Carpenter D, Evoniuk G, et al. (May 2013). "Full central neurokinin-1 receptor blockade is required for efficacy in depression: evidence from orvepitant clinical studies". Journal of Psychopharmacology. 27 (5): 424–434. doi:10.1177/0269881113480990. PMID 23539641. S2CID 6523822.
- ^ Kramer MS, Cutler N, Feighner J, Shrivastava R, Carman J, Sramek JJ, et al. (September 1998). "Distinct mechanism for antidepressant activity by blockade of central substance P receptors". Science. 281 (5383): 1640–1645. Bibcode:1998Sci...281.1640K. doi:10.1126/science.281.5383.1640. PMID 9733503.
- ^ Musselman DL, Miller AH, Porter MR, Manatunga A, Gao F, Penna S, et al. (August 2001). "Higher than normal plasma interleukin-6 concentrations in cancer patients with depression: preliminary findings". The American Journal of Psychiatry. 158 (8): 1252–1257. doi:10.1176/appi.ajp.158.8.1252. PMID 11481159.
- ^ Zhu GF, Chancellor-Freeland C, Berman AS, Kage R, Leeman SE, Beller DI, et al. (June 1996). "Endogenous substance P mediates cold water stress-induced increase in interleukin-6 secretion from peritoneal macrophages". The Journal of Neuroscience. 16 (11): 3745–3752. doi:10.1523/JNEUROSCI.16-11-03745.1996. PMC 6578844. PMID 8642417.
- ^ Clinical trial number NCT02473289 for "An Efficacy and Safety Study of Sirukumab in Participants With Major Depressive Disorder." at ClinicalTrials.gov
- ^ "Sirukumab - Janssen Biotech". AdisInsight. Springer Nature Switzerland AG.
- ^ Peters MC, McGrath KW, Hawkins GA, Hastie AT, Levy BD, Israel E, et al. (July 2016). "Plasma interleukin-6 concentrations, metabolic dysfunction, and asthma severity: a cross-sectional analysis of two cohorts". The Lancet. Respiratory Medicine. 4 (7): 574–584. doi:10.1016/S2213-2600(16)30048-0. PMC 5007068. PMID 27283230.
- ^ Suthaus J, Stuhlmann-Laeisz C, Tompkins VS, Rosean TR, Klapper W, Tosato G, et al. (May 2012). "HHV-8-encoded viral IL-6 collaborates with mouse IL-6 in the development of multicentric Castleman disease in mice". Blood. 119 (22): 5173–5181. doi:10.1182/blood-2011-09-377705. PMC 3370672. PMID 22490805.