Catatonia is a complex neuropsychiatric behavioral syndrome that is characterized by abnormal movements, immobility, abnormal behaviors, and withdrawal.[2][3] The onset of catatonia can be acute or subtle and symptoms can wax, wane, or change during episodes. It has historically been related to schizophrenia (catatonic schizophrenia), but catatonia is most often seen in mood disorders.[3] It is now known that catatonic symptoms are nonspecific and may be observed in other mental, neurological, and medical conditions. Catatonia is now a stand-alone diagnosis (although some experts disagree), and the term is used to describe a feature of the underlying disorder.[4]
| Catatonia | |
|---|---|
| Other names | Catatonic syndrome |
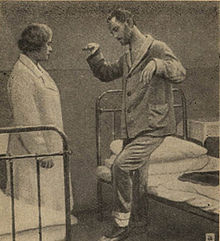 | |
| A patient in catatonic stupor | |
| Specialty | Psychiatry, neurology |
| Symptoms | Immobility, mutism, staring, posturing, rigidity, low consciousness, etc. |
| Complications | Physical trauma, malignant catatonia (autonomic instability, life-threatening), dehydration, pneumonia, pressure ulcers due to immobility, muscle contractions, deep vein thrombosis (DVT)[1] and pulmonary embolism (PE)[1] |
| Causes | Underlying illness (psychiatric, neurologic, or medical), brain injury/damage, certain drugs/medications |
| Diagnostic method | Clinical, Lorazepam challenge |
| Treatment | Benzodiazepines (lorazepam challenge), electroconvulsive therapy (ECT)[1] |
There are several subtypes of catatonia: akinetic catatonia, excited catatonia, malignant catatonia, and delirious mania.[5]
Failure to recognize and treat catatonia may lead to poor outcomes and can be potentially fatal. Treatment with benzodiazepines or ECT can lead to remission of catatonia.[3] There is growing evidence of the effectiveness of the NMDA receptor antagonists amantadine and memantine for benzodiazepine-resistant catatonia.[6] Antipsychotics are sometimes employed, but they can worsen symptoms and have serious adverse effects.[7]
Signs and symptoms edit
The presenting signs of catatonia vary greatly and may be subtle or more markedly pronounced, and symptoms may develop over hours or days to weeks.[8]
Because most patients with catatonia have an underlying psychiatric illness, the majority will present with worsening depression, mania, or psychosis followed by catatonia symptoms.[3] Catatonia presents as a motor disturbance in which patients will display marked reduction in movement, marked agitation, or a mixture of both despite having the physical capacity to move normally. These patients may be unable to start an action or stop one. Movements and mannerisms may be repetitive, or purposeless.[3][9]
The most common signs of catatonia are immobility, mutism, withdrawal and refusal to eat, staring, negativism, posturing (rigidity), rigidity, waxy flexibility/catalepsy, stereotypy (purposeless, repetitive movements), echolalia or echopraxia, verbigeration (repeat meaningless phrases).[10] It should not be assumed that patients presenting with catatonia are unaware of their surroundings as some patients can recall in detail their catatonic state and their actions.[10]
There are several subtypes of catatonia and they are characterized by the specific movement disturbance and associated features. Although catatonia can be divided into various subtypes, the natural history of catatonia is often fluctuant and different states can exist within the same individual.[11]
Subtypes edit
Withdrawn Catatonia: This form of catatonia is characterized by decreased response to external stimuli, immobility or inhibited movement, mutism, staring, posturing, and negativism. Patients may sit or stand in the same position for hours, may hold odd positions, and may resist movement of their extremities.[2][3]
Excited Catatonia: Excited catatonia is characterized by odd mannerisms/gestures, performing purposeless or inappropriate actions, excessive motor activity, restlessness, stereotypy, impulsivity, agitation, and combativeness. Speech and actions may be repetitive or mimic another person's.[2][3][10] People in this state are extremely hyperactive and may have delusions and hallucinations.[12] Catatonic excitement is commonly cited as one of the most dangerous mental states in psychiatry.
Malignant Catatonia: Malignant catatonia is a life-threatening condition that may progress rapidly within a few days. It is characterized by fever, abnormalities in blood pressure, heart rate, respiratory rate, diaphoresis (sweating), and delirium.[2][3] Certain lab findings are common with this presentation; however, they are nonspecific, which means that they are also present in other conditions and do not diagnose catatonia. These lab findings include: leukocytosis, elevated creatine kinase, low serum iron. The signs and symptoms of malignant catatonia overlap significantly with neuroleptic malignant syndrome (NMS) and so a careful history, review of medications, and physical exam are critical to properly differentiate these conditions. For example, if the patient has waxy flexibility and holds a position against gravity when passively moved into that position, then it is likely catatonia. If the patient has a "lead-pipe rigidity" then NMS should be the prime suspect.[citation needed]
Other forms:
- Periodic catatonia is an inconsistently defined entity. In the Wernicke-Kleist-Leonhard school, it is a distinct form of "non-system schizophrenia" characterized by recurrent acute phases with hyperkinetic and akinetic features and often psychotic symptoms, and the build-up of a residual state in between these acute phases, which is characterized by low-level catatonic features and aboulia of varying severity. The condition has a strong hereditary component. According to modern classifications, this may be diagnosed as a form of bipolar disorder, schizoaffective disorder or schizophrenia.[13] Independently, the term periodic catatonia is sometimes used in modern literature to describe a syndrome of recurrent phases of acute catatonia (excited or inhibited type) with full remission between episodes, which resembles the description of "motility psychosis" in the Wernicke-Kleist-Leonhard school.[14]
- System catatonias or systematic catatonias are only defined in the Wernicke-Kleist-Leonhard school. These are chronic-progressive conditions characterized by specific disturbances of volition and psychomotricity, leading to a dramatic decline of executive and adaptive functioning and ability to communicate. They are considered forms of schizophrenia but distinct from other schizophrenic conditions.[14] Affective flattening and apparent loss of interests are common but may be related to reduced emotional expression rather than lack of emotion. Heredity is low. Of the 21 different forms (6 "simple" and 15 "combined" forms) that have been described, most overlap only partially - if at all - with current definitions of either catatonia or schizophrenia, and thus are difficult to classify according to modern diagnostic manuals.[13]
- Early childhood catatonias are also a diagnosis exclusive to the Wernicke-Kleist-Leonhard school, and refers to system catatonias that manifest in young children. Clinically, these conditions resemble severe regressive forms of autism.[13]
- Chronic catatonia-like breakdown or autistic catatonia refers to a functional decline seen in some patients with pre-existing autism spectrum disorder and/or intellectual disability which usually runs a chronic-progressive course and encompasses attenuated catatonic symptoms as well as mood and anxiety symptoms that increasingly interfere with adaptive functioning. Onset is typically insidious and often mistaken for background autistic symptoms. Slowing of voluntary movement, reduced speech, aboulia, increased prompt dependency and obsessive-compulsive symptoms are frequently seen; negativism, (auto-)aggressive behaviors and ill-defined hallucinations have also been reported. Both the causes of this disorder as well as its prognosis appear to be heterogenous, with most patients showing partial recovery upon treatment. It seems to be related to chronic stress as a result of life transitions, loss of external time structuring, sensory sensitivities and/or traumatic experiences, co-morbid mental disorders, or other unknown causes. Since clinical catatonia can not always be diagnosed, this condition has also been renamed to the more general term "late regression".[15][16]
Complications edit
Patients may experience several complications from being in a catatonic state. The nature of these complications will depend on the type of catatonia being experienced by the patient. For example, patients presenting with withdrawn catatonia may have refusal to eat which will in turn lead to malnutrition and dehydration.[17] Furthermore, if immobility is a symptom the patient is presenting with, then they may develop pressure ulcers, muscle contractions, and are at risk of developing deep vein thrombosis (DVT) and pulmonary embolus (PE).[17] Patients with excited catatonia may be aggressive and violent, and physical trauma may result from this. Catatonia may progress to the malignant type which will present with autonomic instability and may be life-threatening. Other complications also include the development of pneumonia and neuroleptic malignant syndrome.[3]
Causes edit
Catatonia is almost always secondary to another underlying illness, often a psychiatric disorder. Mood disorders such as a bipolar disorder and depression are the most common etiologies to progress to catatonia.[3] Other psychiatric associations include schizophrenia and other primary psychotic disorders.[7] It also is related to autism spectrum disorders and ADHD.[18] Psychodynamic theorists have interpreted catatonia as a defense against the potentially destructive consequences of responsibility, and the passivity of the disorder provides relief.[19]
Catatonia is also seen in many medical disorders, including infections (such as encephalitis), autoimmune disorders,[20] meningitis, focal neurological lesions (including strokes),[21] alcohol withdrawal,[22] abrupt or overly rapid benzodiazepine withdrawal,[23][24][25] cerebrovascular disease, neoplasms, head injury,[26] and some metabolic conditions (homocystinuria, diabetic ketoacidosis, hepatic encephalopathy, and hypercalcaemia).[26]
Pathogenesis edit
The pathophysiology that leads to catatonia is still poorly understood and a definite mechanism remains unknown.[10][27] Neurologic studies have implicated several pathways; however, it remains unclear whether these findings are the cause or the consequence of the disorder.[28]
Abnormalities in GABA, glutamate signaling, serotonin, and dopamine transmission are believed to be implicated in catatonia.[3][10][29]
Furthermore, it has also been hypothesized that pathways that connect the basal ganglia with the cortex and thalamus is involved in the development of catatonia.[30]
Diagnosis edit
There is not yet a definitive consensus regarding diagnostic criteria of catatonia. In the fifth edition of the American Psychiatric Association's Diagnostic and Statistical Manual of Mental Disorders (DSM-5, 2013) and the World Health Organization's eleventh edition of the International Classification of Diseases (ICD-11, 2022), the classification is more homogeneous than in earlier editions. Prominent researchers in the field have other suggestions for diagnostic criteria.[31]
DSM-5 classification
The DSM-5 does not classify catatonia as an independent disorder, but rather it classifies it as catatonia associated with another mental disorder, due to another medical condition, or as unspecified catatonia.[32][33] : 134–135
Catatonia is diagnosed by the presence of three or more of the following 12 psychomotor symptoms in association with a mental disorder, medical condition, or unspecified:[32]: 135
- stupor: no psycho-motor activity; not actively relating to the environment
- catalepsy: passive induction of a posture held against gravity
- waxy flexibility: allowing positioning by an examiner and maintaining that position
- mutism: no, or very little, verbal response (exclude if known aphasia)
- negativism: opposition or no response to instructions or external stimuli
- posturing: spontaneous and active maintenance of a posture against gravity
- mannerisms that are odd, circumstantial caricatures of normal actions
- stereotypy: repetitive, abnormally frequent, non-goal-directed movements
- agitation, not influenced by external stimuli
- grimacing: keeping a fixed facial expression
- echolalia: mimicking another's speech
- echopraxia: mimicking another's movements.
Other disorders (additional code 293.89 [F06.1] to indicate the presence of the co-morbid catatonia):
- Catatonia associated with autism spectrum disorder[32]: 57
- Catatonia associated with schizophrenia spectrum and other psychotic disorders
- Catatonia associated with brief psychotic disorder[32]: 109
- Catatonia associated with schizophreniform disorder[32]: 111
- Catatonia associated with schizoaffective disorder[32]: 121
- Catatonia associated with a substance-induced psychotic disorder
- Catatonia associated with bipolar and related disorders[32]: 142
- Catatonia associated with major depressive disorder[32]: 185
- Catatonic disorder due to another medical condition[32]: 136–137
If catatonic symptoms are present but do not form the catatonic syndrome, a medication- or substance-induced aetiology should first be considered.[34]
ICD-11 classification
In ICD-11 catatonia is defined as a syndrome of primarily psychomotor disturbances that is characterized by the simultaneous occurrence of several symptoms such as stupor; catalepsy; waxy flexibility; mutism; negativism; posturing; mannerisms; stereotypies; psychomotor agitation; grimacing; echolalia and echopraxia. Catatonia may occur in the context of specific mental disorders, including mood disorders, schizophrenia or other primary psychotic disorders, and Neurodevelopmental disorders, and may be induced by psychoactive substances, including medications. Catatonia may also be caused by a medical condition not classified under mental, behavioral, or neurodevelopmental disorders.
Assessment/Physical edit
Catatonia is often overlooked and under-diagnosed.[17] Patients with catatonia most commonly have an underlying psychiatric disorder, for this reason, physicians may overlook signs of catatonia due to the severity of the psychosis the patient is presenting with. Furthermore, the patient may not be presenting with the common signs of catatonia such as mutism and posturing. Additionally, the motor abnormalities seen in catatonia are also present in psychiatric disorders. For example, a patient with mania will show increased motor activity that may progress to exciting catatonia. One way in which physicians can differentiate between the two is to observe the motor abnormality. Patients with mania present with increased goal-directed activity. On the other hand, the increased activity in catatonia is not goal-directed and often repetitive.[3]
Catatonia is a clinical diagnosis and there is no specific laboratory test to diagnose it. However, certain testing can help determine what is causing the catatonia. An EEG will likely show diffuse slowing. If seizure activity is driving the syndrome, then an EEG would also be helpful in detecting this. CT or MRI will not show catatonia; however, they might reveal abnormalities that might be leading to the syndrome. Metabolic screens, inflammatory markers, or autoantibodies may reveal reversible medical causes of catatonia.[3]
Vital signs should be frequently monitored as catatonia can progress to malignant catatonia which is life-threatening. Malignant catatonia is characterized by fever, hypertension, tachycardia, and tachypnea.[3]
Rating scale edit
Various rating scales for catatonia have been developed, however, their utility for clinical care has not been well established.[35] The most commonly used scale is the Bush-Francis Catatonia Rating Scale (BFCRS) (external link is provided below).[36] The scale is composed of 23 items with the first 14 items being used as the screening tool. If 2 of the 14 are positive, this prompts for further evaluation and completion of the remaining 9 items.
A diagnosis can be supported by the lorazepam challenge[37] or the zolpidem challenge.[38] While proven useful in the past, barbiturates are no longer commonly used in psychiatry; thus the option of either benzodiazepines or ECT.
Differential diagnosis edit
The differential diagnosis of catatonia is extensive as signs and symptoms of catatonia may overlap significantly with those of other conditions. Therefore, a careful and detailed history, medication review, and physical exam are key to diagnosing catatonia and differentiating it from other conditions. Furthermore, some of these conditions can themselves lead to catatonia. The differential diagnosis is as follows:
- Neuroleptic malignant syndrome (NMS) and catatonia are both life-threatening conditions that share many of the same characteristics including fever, autonomic instability, rigidity, and delirium.[39] Lab values of low serum iron, elevated creatine kinase, and white blood cell count are also shared by the two disorders further complicating the diagnosis. There are features of malignant catatonia (posturing, impulsivity, etc.) that are absent from NMS and the lab results are not as consistent in malignant catatonia as they are in NMS. Some experts consider NMS to be a drug-induced condition associated with antipsychotics, particularly, first generation antipsychotics,[39] but it has not been established as a subtype.[40] Therefore, discontinuing antipsychotics and starting benzodiazepines is a treatment for this condition, and similarly it is helpful in catatonia as well.
- Anti-NMDA receptor encephalitis is an autoimmune disorder characterized by neuropsychiatric features and the presence of IgG antibodies.[41] The presentation of anti-NMDAR encephalitis has been categorized into 5 phases: prodromal phase, psychotic phase, unresponsive phase, hyperkinetic phase, and recovery phase. The psychotic phase progresses into the unresponsive phase characterized by mutism, decreased motor activity, and catatonia.[41]
- Both serotonin syndrome and malignant catatonia may present with signs and symptoms of delirium, autonomic instability, hyperthermia, and rigidity. Again, similar to the presentation in NMS. However, patients with Serotonin syndrome have a history of ingestion of serotonergic drugs (Ex: SSRI). These patients will also present with hyperreflexia, myoclonus, nausea, vomiting, and diarrhea.[42]
- Malignant hyperthermia and malignant catatonia share features of autonomic instability, hyperthermia, and rigidity. However, malignant hyperthermia is a hereditary disorder of skeletal muscle that makes these patients susceptible to exposure to halogenated anesthetics and/or depolarizing muscle relaxants like succinylcholine.[43] Malignant hyperthermia most commonly occurs in the intraoperative or postoperative periods. Other signs and symptoms of malignant hyperthermia include metabolic and respiratory acidosis, hyperkalemia, and cardiac arrhythmias.
- Akinetic mutism is a neurological disorder characterized by a decrease in goal-directed behavior and motivation; however, the patient has an intact level of consciousness.[44] Patients may present with apathy, and may seem indifferent to pain, hunger, or thirst. Akinetic mutism has been associated with structural damage in a variety of brain areas.[45] Akinetic mutism and catatonia may both manifest with immobility, mutism, and waxy flexibility. Differentiating both disorders is the fact that akinetic mutism does not present with echolalia, echopraxia, or posturing. Furthermore, it is not responsive to benzodiazepines as is the case for catatonia.
- Elective mutism has an anxious etiology but has also been associated with personality disorders.[46] Patients with this disorder fail to speak with some individuals but will speak with others. Likewise, they may refuse to speak in certain situations; for example, a child who refuses to speak at school but is conversational at home. This disorder is distinguished from catatonia by the absence of any other signs/symptoms.
- Nonconvulsive status epilepticus is seizure activity with no accompanying tonic-clonic movements.[47] It can present with stupor, similar to catatonia, and they both respond to benzodiazepines. Nonconvulsive status epilepticus is diagnosed by the presence of seizure activity seen on electroencephalogram (EEG).[48] Catatonia on the other hand, is associated with normal EEG or diffuse slowing.
- Delirium is characterized by fluctuating disturbed perception and consciousness in the ill individual.[49] It has hypoactive and hyperactive or mixed forms. People with hyperactive delirium present similarly to those with excited catatonia and have symptoms of restlessness, agitation, and aggression. Those with hypoactive delirium present with similarly to retarded catatonia, withdrawn and quiet. However, catatonia also includes other distinguishing features including posturing and rigidity as well as a positive response to benzodiazepines.
- Patients with locked-in syndrome present with immobility and mutism; however, unlike patients with catatonia who are unmotivated to communicate, patients with locked-in syndrome try to communicate with eye movements and blinking. Furthermore, locked-in syndrome is caused by damage to the brainstem.[50]
- Stiff-person syndrome and catatonia are similar in that they may both present with rigidity, autonomic instability and a positive response to benzodiazepines.[51] However, stiff-person syndrome may be associated with anti-glutamic acid decarboxylase (anti-GAD) antibodies[52][53] and other catatonic signs such as mutism and posturing are not part of the syndrome.
- Untreated late-stage Parkinson's disease may present similarly to retarded catatonia with symptoms of immobility, rigidity, and difficulty speaking. Further complicating the diagnosis is the fact that many patients with Parkinson's disease will have major depressive disorder, which may be the underlying cause of catatonia. Parkinson's disease can be distinguished from catatonia by a positive response to levodopa. Catatonia on the other hand will show a positive response to benzodiazepines.
- Extrapyramidal side effects of antipsychotic medication, especially dystonia and akathisia, can be difficult to distinguish from catatonic symptoms, or may confound them in the psychiatric setting. Extrapyramidal motor disorders usually do not involve social symptoms like negativism, while individuals with catatonic excitement typically do not have the physically painful compulsion to move that is seen in akathisia.[54]
- Certain stimming behaviors and stress responses in individuals with autism spectrum disorders can present similarly to catatonia. In autism spectrum disorders, chronic catatonia is distinguished by a lasting deterioration of adaptive skills from the background of pre-existing autistic symptomatology that cannot be easily explained. Acute catatonia is usually clearly distinguishable from autistic symptoms.[16]
- The diagnostic entities of obsessional slowness and psychogenic parkinsonism show overlapping features with catatonia, such as motor slowness, gegenhalten (oppositional paratonia), mannerisms, and reduced or absent speech. However, psychogenic parkinsonism involves tremor which is unusual in catatonia.[55] Obsessional slowness is a controversial diagnosis, with presentations ranging from severe but common manifestations of obsessive compulsive disorder to catatonia.[56]
- Down Syndrome Disintegrative Disorder (or Down Syndrome Regression Disorder, DSDD / DSRD) is a chronic condition characterized by loss of previously acquired adaptive, cognitive and social functioning occurring in persons with Down Syndrome, usually during adolescence or early adulthood. The clinical picture is variable, but often includes catatonic signs, which is why it was called "catatonic psychosis" in initial reports in 1946.[57] DSDD seems to phenotypically overlap with obsessional slowness (see above)[58] and catatonia-like regression occurring in ASD.[59]
Treatment edit
The initial treatment of catatonia is to stop medication that could be potentially leading to the syndrome.[37] These may include steroids, stimulants, anticonvulsants, neuroleptics or dopamine blockers.[3] A "lorazepam challenge", in which patients are given 2 mg of IV lorazepam (or another benzodiazepine) may aid in the diagnosis.[60] Most patients with catatonia will respond significantly to this within the first 15–30 minutes. If no change is observed during the first dose, then a second dose is given and the patient is re-examined. If the patient responds to the lorazepam challenge, then lorazepam can be scheduled at interval doses until the catatonia resolves.[3] The lorazepam must be tapered slowly, otherwise, the catatonia symptoms may return. The underlying cause of the catatonia should also be treated during this time. ECT may also be used to resolve catatonia. The success rate of ECT and lorazepam in the treatment of catatonia is estimated to be 60-100%, with earlier treatment being associated with a greater likelihood of treatment success.[8] ECT is usually administered as multiple sessions over one-two weeks and is usually successful in those in which lorazepam fails.[8] ECT in combination with benzodiazepines is used to treat malignant catatonia. In France, zolpidem has also been used in diagnosis, and response may occur within the same time period. Ultimately the underlying cause needs to be treated.[7]
Supportive care is required in those with catatonia. This includes monitoring vital signs and fluid status, and in those with chronic symptoms; maintaining nutrition and hydration, medications to prevent a blood clot, and measures to prevent the development of pressure ulcers.[8]
Electroconvulsive therapy (ECT) is an effective treatment for catatonia that is well acknowledged.[37] ECT has also shown favorable outcomes in patients with chronic catatonia. However, it has been pointed out that further high quality randomized controlled trials are needed to evaluate the efficacy, tolerance, and protocols of ECT in catatonia.[61]
Antipsychotics are sometimes used in those with a co-existing psychosis, however they should be used with care as they may worsen catatonia and have a risk of neuroleptic malignant syndrome, a dangerous condition that can mimic catatonia and requires immediate discontinuation of the antipsychotic.[7][8]
There is evidence that clozapine works better than other antipsychotics to treat catatonia.[62][8]
Excessive glutamate activity is believed to be involved in catatonia;[62] when first-line treatment options fail, NMDA antagonists such as amantadine or memantine may be used. Amantadine may have an increased incidence of tolerance with prolonged use and can cause psychosis, due to its additional effects on the dopamine system. Memantine has a more targeted pharmacological profile for the glutamate system, reduced incidence of psychosis and may therefore be preferred for individuals who cannot tolerate amantadine. Topiramate is another treatment option for resistant catatonia; it produces its therapeutic effects by producing glutamate antagonism via modulation of AMPA receptors.[6]
Prognosis edit
Twenty-five percent of psychiatric patients with catatonia will have more than one episode throughout their lives.[8] Treatment response for patients with catatonia is 50–70%, with treatment failure being associated with a poor prognosis. Many of these patients will require long-term and continuous mental health care. For patients with catatonia with underlying schizophrenia, the prognosis is much poorer.[3]
Epidemiology edit
Catatonia has been historically studied in psychiatric patients.[63] Catatonia is underrecognized and the features may be mistaken for other disorders (such as negative symptoms of schizophrenia), leading to an underestimate of the prevalence. The prevalence has been reported to be as high as 10% in those with acute psychiatric illnesses, and 9-30% in the setting of inpatient psychiatric care.[8][64][10] One large population estimate has suggested that the incidence of catatonia is 10.6 episodes per 100 000 person-years.[65] It occurs in males and females in approximately equal numbers.[66][65] 21-46% of all catatonia cases can be attributed to a general medical condition.[17]
History edit
Reports of stupor-like and catatonia-like states abound in the history of psychiatry.[67] After the middle of the 19th century there was an increase of interest in the motor disorders accompanying madness,[68] culminating in the publication by Karl Ludwig Kahlbaum in 1874 of Die Katatonie oder das Spannungsirresein ("Catatonia or Tension Insanity").[69]
See also edit
- Acquiescence
- Akinetic mutism
- Autistic catatonia
- Awakenings (1990 biopic about catatonic patients, based on Oliver Sacks's book of the same name)
- Blank expression
- Botulism
- Clouding of consciousness
- Disorganized schizophrenia
- Homecoming (features catatonia as a main plot point)
- Karolina Olsson
- Oneiroid syndrome
- Paranoid schizophrenia
- Persistent vegetative state
- Resignation syndrome
- Sensory overload
- Tonic immobility
- Sleep paralysis
References edit
- ^ a b c Balaguer AP, Rivero IS (22 December 2021). "Electroconvulsive therapy, catatonia, deep vein thrombosis and anticoagulant treatment: a case report". General Psychiatry. 34 (6): e100666. doi:10.1136/gpsych-2021-100666. ISSN 2517-729X. PMC 8705197. PMID 35028525.
- ^ a b c d Fink M, Taylor MA (1 November 2009). "The Catatonia Syndrome: Forgotten but Not Gone". Archives of General Psychiatry. 66 (11): 1173–1177. doi:10.1001/archgenpsychiatry.2009.141. PMID 19884605.
- ^ a b c d e f g h i j k l m n o p q Burrow JP, Spurling BC, Marwaha R (2022). "Catatonia". StatPearls. StatPearls Publishing. PMID 28613592.
- ^ Fink M (2011). "Catatonia from its creation to DSM-V: Considerations for ICD". Indian Journal of Psychiatry. 53 (3): 214–217. doi:10.4103/0019-5545.86810. PMC 3221176. PMID 22135438.
- ^ Fink M (July 2009). "Catatonia: A Syndrome Appears, Disappears, and is Rediscovered". The Canadian Journal of Psychiatry. 54 (7): 437–445. doi:10.1177/070674370905400704. PMID 19660165.
- ^ a b Carroll BT, Goforth HW, Thomas C, Ahuja N, McDaniel WW, Kraus MF, Spiegel DR, Franco KN, Pozuelo L, Muñoz C (October 2007). "Review of Adjunctive Glutamate Antagonist Therapy in the Treatment of Catatonic Syndromes". The Journal of Neuropsychiatry and Clinical Neurosciences. 19 (4): 406–412. doi:10.1176/jnp.2007.19.4.406. PMID 18070843.
- ^ a b c d Fink M, Taylor MA (2003). Catatonia: A Clinician's Guide to Diagnosis and Treatment. Cambridge University Press. ISBN 978-0-521-82226-8.[page needed]
- ^ a b c d e f g h Heckers S, Walther S (9 November 2023). "Catatonia". New England Journal of Medicine. 389 (19): 1797–1802. doi:10.1056/NEJMra2116304. PMID 37937779. S2CID 265673511.
- ^ Zisselman MH, Jaffe RL (February 2010). "ECT in the Treatment of a Patient With Catatonia: Consent and Complications". American Journal of Psychiatry. 167 (2): 127–132. doi:10.1176/appi.ajp.2009.09050703. PMID 20123920.
- ^ a b c d e f Rasmussen SA, Mazurek MF, Rosebush PI (2016). "Catatonia: Our current understanding of its diagnosis, treatment and pathophysiology". World Journal of Psychiatry. 6 (4): 391–398. doi:10.5498/wjp.v6.i4.391. PMC 5183991. PMID 28078203.
- ^ Shorter E, Fink M (2018). The Madness of Fear: A History of Catatonia. Oxford University Press. ISBN 978-0-19-088119-1.
- ^ Nolen-Hoeksema S (2014). Abnormal Psychology. McGraw-Hill Education. p. 224. ISBN 978-1-259-06072-4.
- ^ a b c "Cercle d'excellence sur les Psychoses: Introduction". www.cercle-d-excellence-psy.org. Retrieved 25 May 2022.[permanent dead link]
- ^ a b Gazdag G, Takács R, Ungvari GS (22 September 2017). "Catatonia as a putative nosological entity: A historical sketch". World Journal of Psychiatry. 7 (3): 177–183. doi:10.5498/wjp.v7.i3.177. PMC 5632602. PMID 29043155.
- ^ Ghaziuddin M (28 October 2021). "Catatonia: A Common Cause of Late Regression in Autism". Frontiers in Psychiatry. 12: 674009. doi:10.3389/fpsyt.2021.674009. PMC 8585308. PMID 34777033.
- ^ a b Vaquerizo-Serrano J, Salazar De Pablo G, Singh J, Santosh P (2022). "Catatonia in autism spectrum disorders: A systematic review and meta-analysis". European Psychiatry. 65 (1): e4. doi:10.1192/j.eurpsy.2021.2259. PMC 8792870. PMID 34906264.
- ^ a b c d Serra-Mestres J, Jaimes-Albornoz W (29 June 2018). "Recognizing Catatonia in Medically Hospitalized Older Adults: Why It Matters". Geriatrics. 3 (3): 37. doi:10.3390/geriatrics3030037. PMC 6319219. PMID 31011075.
- ^ Dhossche DM, Rout U (2006). "Are Autistic and Catatonic Regression Related? A Few Working Hypotheses Involving Gaba, Purkinje Cell Survival, Neurogenesis, and ECT". International Review of Neurobiology. Vol. 72. pp. 55–79. doi:10.1016/S0074-7742(05)72004-3. ISBN 978-0-12-366873-8. PMID 16697291.
- ^ Arieti S (1994). Interpretation of schizophrenia. Jason Aronson. ISBN 1-56821-209-7. OCLC 472906047.
- ^ Rogers JP, Pollak TA, Blackman G, David AS (July 2019). "Catatonia and the immune system: a review". The Lancet Psychiatry. 6 (7): 620–630. doi:10.1016/S2215-0366(19)30190-7. PMC 7185541. PMID 31196793.
- ^ Haroche A, Rogers J, Plaze M, Gaillard R, Williams SC, Thomas P, Amad A (July 2020). "Brain imaging in catatonia: systematic review and directions for future research". Psychological Medicine. 50 (10): 1585–1597. doi:10.1017/S0033291720001853. PMID 32539902. S2CID 219704600.
- ^ Geoffroy PA, Rolland B, Cottencin O (1 May 2012). "Catatonia and Alcohol Withdrawal: A Complex and Underestimated Syndrome". Alcohol and Alcoholism. 47 (3): 288–290. doi:10.1093/alcalc/agr170. PMID 22278315.
- ^ Rosebush PI, Mazurek MF (August 1996). "Catatonia after benzodiazepine withdrawal". Journal of Clinical Psychopharmacology. 16 (4): 315–319. doi:10.1097/00004714-199608000-00007. PMID 8835707.
- ^ Deuschle M, Lederbogen F (January 2001). "Benzodiazepine withdrawal-induced catatonia". Pharmacopsychiatry. 34 (1): 41–42. doi:10.1055/s-2001-15188. PMID 11229621. S2CID 260241781.
- ^ Kanemoto K, Miyamoto T, Abe R (September 1999). "Ictal catatonia as a manifestation of de novo absence status epilepticus following benzodiazepine withdrawal". Seizure. 8 (6): 364–366. doi:10.1053/seiz.1999.0309. PMID 10512781. S2CID 17454162.
- ^ a b American Psychiatric Association (2013). Diagnostic and Statistical Manual of Mental Disorders (Fifth ed.). Arlington, VA: American Psychiatric Publishing. pp. 119–121. ISBN 978-0-89042-555-8.
- ^ Walther S, Stegmayer K, Wilson JE, Heckers S (July 2019). "Structure and neural mechanisms of catatonia". The Lancet Psychiatry. 6 (7): 610–619. doi:10.1016/S2215-0366(18)30474-7. PMC 6790975. PMID 31196794.
- ^ Dhossche DM, Stoppelbein L, Rout UK (December 2010). "Etiopathogenesis of Catatonia: Generalizations and Working Hypotheses". The Journal of ECT. 26 (4): 253–258. doi:10.1097/YCT.0b013e3181fbf96d. PMID 21076339.
- ^ Northoff G (July 2000). "Brain Imaging in Catatonia: Current Findings and a Pathophysiologic Model". CNS Spectrums. 5 (7): 34–46. doi:10.1017/s1092852900013377. PMID 18197154. S2CID 12837559.
- ^ Northoff G (October 2002). "What catatonia can tell us about 'top-down modulation': A neuropsychiatric hypothesis". Behavioral and Brain Sciences. 25 (5): 555–577. doi:10.1017/s0140525x02000109. PMID 12958742. S2CID 20407002.
- ^ Fink M (2003). Catatonia : a clinician's guide to diagnosis and treatment. Michael Alan Taylor. Cambridge: Cambridge University Press. ISBN 0-511-06198-6. OCLC 57254202.[page needed]
- ^ a b c d e f g h i American Psychiatric Association (2022). Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition, Text Revision. Washington, DC: American Psychiatric Association. doi:10.1176/appi.books.9780890425787. ISBN 978-0-89042-575-6. S2CID 249488050.
- ^ Jeste DV, Lieberman JA, Benson RS, Young ML, Akaka J, Bernstein CA, Crowley B, Everett AS, Geller J, Graff MD, Greene JA, Kashtan JF, Mcvoy MK, Nininger JE, Oldham JM, Schatzberg AF, Widge AS, Vanderlip ER (2013). Diagnostic and Statistical Manual of Mental Disorders Fifth Edition DSM-5TM. American Psychiatric Association. Retrieved 8 December 2023.
- ^ Michael B. First (2013). DSM-5® Handbook of Differential Diagnosis. American Psychiatric Publishing. p. 49. ISBN 978-1-58562-998-5.
- ^ Sienaert P, Rooseleer J, De Fruyt J (December 2011). "Measuring catatonia: A systematic review of rating scales". Journal of Affective Disorders. 135 (1–3): 1–9. doi:10.1016/j.jad.2011.02.012. PMID 21420736.
- ^ Bush G, Fink M, Petrides G, Dowling F, Francis A (February 1996). "Catatonia. I. Rating scale and standardized examination". Acta Psychiatrica Scandinavica. 93 (2): 129–136. doi:10.1111/j.1600-0447.1996.tb09814.x. PMID 8686483. S2CID 20752576.
- ^ a b c Sienaert P, Dhossche DM, Vancampfort D, De Hert M, Gazdag G (9 December 2014). "A Clinical Review of the Treatment of Catatonia". Frontiers in Psychiatry. 5: 181. doi:10.3389/fpsyt.2014.00181. PMC 4260674. PMID 25538636.
- ^ "Catatonia in French Psychiatry: Implications of the Zolpidem Challenge Test". Psychiatric Annals. 37 (1): 00485713–20070101–02. January 2007. doi:10.3928/00485713-20070101-02.
- ^ a b Simon LV, Hashmi MF, Callahan AL (2022). "Neuroleptic Malignant Syndrome". StatPearls. StatPearls Publishing. PMID 29489248.
- ^ Northoff G (1 December 2002). "Catatonia and neuroleptic malignant syndrome: psychopathology and pathophysiology". Journal of Neural Transmission. 109 (12): 1453–1467. CiteSeerX 10.1.1.464.9266. doi:10.1007/s00702-002-0762-z. PMID 12486486. S2CID 12971112.
- ^ a b Samanta D, Lui F (2022). "Anti-NMDA Receptor Encephalitis". StatPearls. StatPearls Publishing. PMID 31869136.
- ^ Foong AL, Grindrod KA, Patel T, Kellar J (October 2018). "Demystifying serotonin syndrome (or serotonin toxicity)". Canadian Family Physician. 64 (10): 720–727. PMC 6184959. PMID 30315014.
- ^ Watt S, McAllister RK (2022). "Malignant Hyperthermia". StatPearls. StatPearls Publishing. PMID 28613578.
- ^ Arnts H, van Erp WS, Lavrijsen JC, van Gaal S, Groenewegen HJ, van den Munckhof P (May 2020). "On the pathophysiology and treatment of akinetic mutism". Neuroscience & Biobehavioral Reviews. 112: 270–278. doi:10.1016/j.neubiorev.2020.02.006. hdl:11245.1/c438b878-4d5b-4f13-887c-7f01df095324. PMID 32044373.
- ^ Ackermann H, Ziegler W (February 1995). "Akinetischer Mutismus – eine Literaturübersicht". Fortschritte der Neurologie · Psychiatrie. 63 (2): 59–67. doi:10.1055/s-2007-996603. PMID 7705740. S2CID 260156218.
- ^ Holka-Pokorska J, Piróg-Balcerzak A, Jarema M (30 April 2018). "The controversy around the diagnosis of selective mutism – a critical analysis of three cases in the light of modern research and diagnostic criteria". Psychiatria Polska. 52 (2): 323–343. doi:10.12740/PP/76088. PMID 29975370.
- ^ Wylie T, Sandhu DS, Murr N (2022). "Status Epilepticus". StatPearls. StatPearls Publishing. PMID 28613459.
- ^ Sutter R, Kaplan PW (August 2012). "Electroencephalographic criteria for nonconvulsive status epilepticus: Synopsis and comprehensive survey: EEG Criteria for NCSE". Epilepsia. 53: 1–51. doi:10.1111/j.1528-1167.2012.03593.x. PMID 22862158. S2CID 24014621.
- ^ Delirium: prevention, diagnosis and management. National Institute for Health and Care Excellence: Guidelines. National Institute for Health and Care Excellence (NICE). 2019. ISBN 978-1-4731-2992-4. PMID 31971702.
- ^ M Das J, Anosike K, Asuncion RM (2022). "Locked-in Syndrome". StatPearls. StatPearls Publishing. PMID 32644452.
- ^ Balint B, Meinck HM (July 2018). "Pragmatic Treatment of Stiff Person Spectrum Disorders: Pragmatic Treatment of SPSD". Movement Disorders Clinical Practice. 5 (4): 394–401. doi:10.1002/mdc3.12629. PMC 6174384. PMID 30363317.
- ^ Baizabal-Carvallo JF, Jankovic J (August 2015). "Stiff-person syndrome: insights into a complex autoimmune disorder". Journal of Neurology, Neurosurgery & Psychiatry. 86 (8): 840–848. doi:10.1136/jnnp-2014-309201. PMID 25511790. S2CID 19981869.
- ^ Sarva H, Deik A, Ullah A, Severt WL (4 March 2016). "Clinical Spectrum of Stiff Person Syndrome: A Review of Recent Reports". Tremor and Other Hyperkinetic Movements. 6: 340. doi:10.7916/D85M65GD. PMC 4790195. PMID 26989571.
- ^ Rasmussen SA, Mazurek MF, Rosebush PI (2016). "Catatonia: Our current understanding of its diagnosis, treatment and pathophysiology". World Journal of Psychiatry. 6 (4): 1875–1879. doi:10.5498/wjp.v6.i4.391. PMC 5183991. PMID 8078203.
- ^ Thenganatt M, Jankovic J (2016). "Psychogenic (Functional) parkinsonism". Functional Neurologic Disorders. Handbook of Clinical Neurology. Vol. 139. pp. 259–262. doi:10.1016/B978-0-12-801772-2.00022-9. ISBN 978-0-12-801772-2. PMID 27719845.
- ^ Ganos C, Kassavetis P, Cerdan M, Erro R, Balint B, Price G, Edwards MJ, Bhatia KP (June 2015). "Revisiting the Syndrome of "Obsessional Slowness"". Movement Disorders Clinical Practice. 2 (2): 163–169. doi:10.1002/mdc3.12140. PMC 6353487. PMID 30713890. S2CID 73414098.
- ^ Rosso M, Fremion E, Santoro SL, Oreskovic NM, Chitnis T, Skotko BG, Santoro JD (2020). "Down Syndrome Disintegrative Disorder: A Clinical Regression Syndrome of Increasing Importance". Pediatrics. 145 (6): e20192939. doi:10.1542/peds.2019-2939. PMID 32471843. S2CID 219104019.
- ^ https://adscresources.advocatehealth.com/resources/obsessional-slowness/#:~:text=The%20persistent%20stress%20of%20the%20rapidly%20moving%20environment,slowness%2C%20which%20we%20have%20also%20labeled%20%E2%80%9CThe%20Pace.%E2%80%9D; retrieved 2023 Aug 18
- ^ Lyons A, Allen NM, Flanagan O, Cahalane D (2020). "Catatonia as a feature of down syndrome: An under-recognised entity?". European Journal of Paediatric Neurology. 25: 187–190. doi:10.1016/j.ejpn.2020.01.005. PMID 31959555. S2CID 210841869.
- ^ Daniels J (October 2009). "Catatonia: Clinical Aspects and Neurobiological Correlates". The Journal of Neuropsychiatry and Clinical Neurosciences. 21 (4): 371–380. doi:10.1176/jnp.2009.21.4.371. PMID 19996245.
- ^ Leroy A, Naudet F, Vaiva G, Francis A, Thomas P, Amad A (October 2018). "Is electroconvulsive therapy an evidence-based treatment for catatonia? A systematic review and meta-analysis". European Archives of Psychiatry and Clinical Neuroscience. 268 (7): 675–687. doi:10.1007/s00406-017-0819-5. PMID 28639007. S2CID 4013882.
- ^ a b Saini A, Begum N, Matti J, Ghanem DA, Fripp L, Pollak TA, Zandi MS, David A, Lewis G, Rogers J (15 September 2022). "Clozapine as a treatment for catatonia: A systematic review" (PDF). Schizophrenia Research. 263: 275–281. doi:10.1016/j.schres.2022.09.021. ISSN 0920-9964. PMID 36117082. S2CID 252276294.
- ^ American Psychiatric Association (2022). Diagnostic and Statistical Manual of Mental Disorders. doi:10.1176/appi.books.9780890425787. ISBN 978-0-89042-578-7. S2CID 249488050.[page needed]
- ^ Solmi M, Pigato GG, Roiter B, Guaglianone A, Martini L, Fornaro M, Monaco F, Carvalho AF, Stubbs B, Veronese N, Correll CU (20 August 2018). "Prevalence of Catatonia and Its Moderators in Clinical Samples: Results from a Meta-analysis and Meta-regression Analysis". Schizophrenia Bulletin. 44 (5): 1133–1150. doi:10.1093/schbul/sbx157. PMC 6101628. PMID 29140521.
- ^ a b Rogers JP, Pollak TA, Begum N, Griffin A, Carter B, Pritchard M, Broadbent M, Kolliakou A, Ke J, Stewart R, Patel R, Bomford A, Amad A, Zandi MS, Lewis G, Nicholson TR, David AS (2 November 2021). "Catatonia: demographic, clinical and laboratory associations". Psychological Medicine. 53 (6): 2492–2502. doi:10.1017/S0033291721004402. PMC 10123832. PMID 35135642. S2CID 242076501.
- ^ Parsanoglu Z, Balaban OD, Gica S, Atay OC, Altin O (May 2022). "Comparison of the Clinical and Treatment Characteristics of Patients Undergoing Electroconvulsive Therapy for Catatonia Indication in the Context of Gender". Clinical EEG and Neuroscience. 53 (3): 175–183. doi:10.1177/15500594211025889. PMID 34142904. S2CID 235471133.
- ^ Berrios GE (1981). "Stupor: A conceptual history". Psychological Medicine. 11 (4): 677–688. doi:10.1017/s0033291700041179. PMID 7034030. S2CID 26932116.
- ^ Berrios GE, Marková IS (2018). "Historical and conceptual aspects of motor disorders in the psychoses". Schizophrenia Research. 200: 5–11. doi:10.1016/j.schres.2017.09.008. PMID 28941779. S2CID 26892840.
- ^ "Zur Entwicklung der Psychiatrie - ein Internet-Atlas von Dr. Hans-Peter Haack" (in German). Archived from the original on 9 February 2008. Retrieved 29 June 2017.
External links edit
- Catatonia in DSM-5
- Encyclopedia of Mental Disorders – Catatonic Disorders
- "Schizophrenia: Catatonic Type" video by Heinz Edgar Lehmann, 1952
- Bush-Francis Catatonia Rating Scale