| Prolactinoma | |
|---|---|
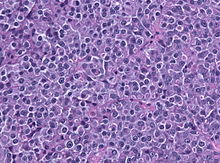 | |
| Specialty | Endocrinology, neurosurgery[1] |
| Symptoms | High prolactin: sexual dysfunction in males; decreased periods, infertility, milk production in females; decreased growth in children[1] Pressure effects: visual field defects, cranial nerve palsy, headaches[1] |
| Complications | Seizures, pituitary apoplexy[1] |
| Usual onset | Around 30 years[1] |
| Types | Micro, macro, giant[1] |
| Causes | Generally unclear[1] |
| Risk factors | Family history, multiple endocrine neoplasia type 1[1] |
| Diagnostic method | Based on lab tests and medical imaging after ruling out other causes[1] |
| Differential diagnosis | Pregnancy, certain medications, hypothyroidism[1] |
| Treatment | Periodically monitored, cabergoline, bromocriptine, hormone replacement therapy, surgery, radiation therapy[1] |
| Prognosis | Small (excellent), larger (mixed)[1] |
| Frequency | 2 per 10,000 people[1] |
A prolactinoma is a benign tumor of the pituitary gland that produces the hormone prolactin.[1] Symptoms result from high prolactin levels or pressure on surrounding tissues.[1] High prolactin can result in sexual dysfunction in males; decreased periods, infertility, and milk production in females; and decreased growth in children.[1] Pressure effects may include visual field defects, cranial nerve palsy, and headaches.[1] Complications may include seizures or pituitary apoplexy.[1]
The cause in most cases is unclear.[1][2] Risk factors include family history and multiple endocrine neoplasia type 1.[1] Diagnosis is based on lab tests and medical imaging after ruling out other possible causes.[1] They are classified into micro- (<10 mm diameter), macro- (10 to 40 mm diameter), and giant (>40 mm diameter).[1]
Small prolactinomas without symptoms may be simply periodically monitored.[1] Large or symptomatic cases may be treated with cabergoline and bromocriptine.[1] Hormone replacement therapy may also be used.[1] If this is not successful surgery or radiation therapy may be used.[1] Outcomes for small prolactinomas are generally excellent, while that of larger lesions is mixed.[1]
Prolactinomas affected about 2 per 10,000 people.[1] They are three times more common in women than men.[1] Onset is often around 30 years of age.[1] It is the most common type of functioning pituitary tumor.[3] Prolactinomas were first clearly described in the 1950s and 1960s.[4][5]
References
edit- ^ a b c d e f g h i j k l m n o p q r s t u v w x y z aa ab ac ad Yatavelli, RKR; Bhusal, K (January 2020). "Prolactinoma". PMID 29083585.
{{cite journal}}: Cite journal requires|journal=(help) - ^ "Prolactinoma | NIDDK". National Institute of Diabetes and Digestive and Kidney Diseases. Archived from the original on 28 January 2021. Retrieved 21 January 2021.
- ^ Glezer A, Bronstein MD (2015). "Prolactinomas". Endocrinol Metab Clin North Am. 44 (1): 71–78. doi:10.1016/j.ecl.2014.11.003. PMID 25732643.
- ^ Kronenberg, Henry (2007). Williams Textbook of Endocrinology. Elsevier Health Sciences. p. 186. ISBN 978-1-4377-2181-2. Archived from the original on 2021-08-29. Retrieved 2021-01-21.
- ^ Welbourn, Richard Burkewood; Friesen, Stanley R.; Johnston, Ivan D. A.; Sellwood, Ronald A. (1990). The History of Endocrine Surgery. Greenwood Publishing Group. p. 115. ISBN 978-0-275-92586-4. Archived from the original on 2021-08-29. Retrieved 2021-01-21.