Typhus, also known as typhus fever, is a group of infectious diseases that include epidemic typhus, scrub typhus, and murine typhus.[1] Common symptoms include fever, headache, and a rash.[1] Typically these begin one to two weeks after exposure.[2]
| Typhus | |
|---|---|
| Other names | Typhus fever |
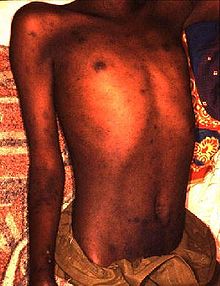 | |
| Rash caused by epidemic typhus | |
| Specialty | Infectious disease |
| Symptoms | Fever, headache, rash[1] |
| Complications | Meningoencephalitis |
| Usual onset | 1–2 weeks after exposure[2] |
| Causes | Bacterial infection spread by parasites[1] |
| Risk factors | Poor sanitation |
| Prevention | Avoiding exposure to organisms known to carry the disease |
| Treatment | Doxycycline[2] |
| Frequency | Rare[3] |
The diseases are caused by specific types of bacterial infection.[1] Epidemic typhus is caused by Rickettsia prowazekii spread by body lice, scrub typhus is caused by Orientia tsutsugamushi spread by chiggers, and murine typhus is caused by Rickettsia typhi spread by fleas.[1]
Vaccines have been developed, but none are commercially available.[3][4][5] Prevention is achieved by reducing exposure to the organisms that spread the disease.[3][4][5] Treatment is with the antibiotic doxycycline.[2] Epidemic typhus generally occurs in outbreaks when poor sanitary conditions and crowding are present.[6] While once common, it is now rare.[3] Scrub typhus occurs in Southeast Asia, Japan, and northern Australia.[4] Murine typhus occurs in tropical and subtropical areas of the world.[5]
Typhus has been described since at least 1528.[7] The name comes from the Greek tûphos (τῦφος), meaning hazy or smoky and commonly used as a word for delusion, describing the state of mind of those infected.[7] While "typhoid" means "typhus-like", typhus and typhoid fever are distinct diseases caused by different types of bacteria.[8] Note, however, that in some languages such as German, the term typhus does mean the "typhoid fever", caused by specific strains of Salmonella typhi bacteria, and the here depicted "typhus" is called lice fever.
Signs and symptoms edit
These signs and symptoms refer to epidemic typhus, as it is the most important of the typhus group of diseases.[9]
Signs and symptoms begin with sudden onset of fever and other flu-like symptoms about one to two weeks after being infected.[10] Five to nine days after the symptoms have started, a rash typically begins on the trunk and spreads to the extremities. This rash eventually spreads over most of the body, sparing the face, palms, and soles. Signs of meningoencephalitis begin with the rash and continue into the second or third weeks.[citation needed] Other signs of meningoencephalitis include sensitivity to light (photophobia), altered mental status (delirium), or coma. Untreated cases are often fatal.[11]
Signs and symptoms of scrub typhus usually start within 1 to 2 weeks after being infected. These symptoms include fever, headaches, chills, swollen lymph nodes, nausea/vomiting, and a rash at the site of infection called an eschar. More severe symptoms may damage the lungs, brain, kidney, meninges, and heart.[12]
Causes edit
Multiple diseases include the word "typhus" in their descriptions.[13] Types include:
| Condition | Bacterium | Reservoir/vector | Notes |
|---|---|---|---|
| Epidemic louse-borne typhus | Rickettsia prowazekii | Body louse | When the term "typhus" is used without qualification, this is usually the condition described. Historical references to "typhus" are now generally considered to be this condition.[citation needed] |
| Murine typhus or "endemic typhus" | Rickettsia typhi | Fleas on rats | |
| Scrub typhus | Orientia tsutsugamushi | Harvest mites on humans or rodents | |
| Spotted fever | Rickettsia spotted fever group | Ticks | Includes Boutonneuse fever, Rocky Mountain spotted fever, Queensland tick typhus and other variants. |
Diagnosis edit
The main method of diagnosing typhus of all types is laboratory testing. It is most commonly done with an indirect immunofluorescence antibody IFA test for all types of typhus. This tests a sample for the antibodies associated with typhus. It can also be done with either immunohistochemistry (IHC) or polymerase chain reaction (PCR) tests excluding scrub typhus. Scrub typhus is not tested with IHC or PCR but is instead tested with the IFA test as well as indirect immunuoperoxidase (IIP) assays.[14]
Prevention edit
As of 2024, no vaccine is commercially available.[3][4][5] A vaccine has been in development for scrub typhus known as the scrub typhus vaccine.[15]
Scrub typhus edit
Scrub typhus is caused by mites, so avoid the outdoors when scrub is common in the area. Make sure your clothing is treated with permethrin to prevent mite bites. Lastly, make sure to use bug spray to keep mites away as well. For children and babies, you additionally have to make sure their clothing covers their limbs. For babies put a mosquito cover over their stroller which also protects them from mites.[16]
Epidemic typhus edit
Epidemic typhus is caused by body lice and thrives in areas with overcrowding. To avoid lice you should stay away from highly populated areas. Also, make sure to regularly clean yourself and your clothing to help kill louse. This also goes for things like bedding and towels. Make sure to not share any fabric items with anyone who has lice or typhus. Lastly, treat clothing with permethrin because it helps kill lice.[3]
Murine typhus edit
Murine typhus is caused by flea bites so take steps to avoid fleas. This can be done by making sure pets do not have fleas and if they do, treat them, stay away from wild animals, use insect repellent to keep fleas away, and wear gloves when dealing with sick or dead animals. Take steps to ensure rodents or other wildlife do not get into your home.[17]
Treatment edit
The American Public Health Association recommends treatment based upon clinical findings and before culturing confirms the diagnosis.[18] Without treatment, death may occur in 10% to 60% of people with epidemic typhus, with people over age 50 having the highest risk of death.[19] In the antibiotic era, death is uncommon if doxycycline is given. In one study of 60 people hospitalized with epidemic typhus, no one died when given doxycycline or chloramphenicol.[20]
Epidemiology edit
According to the World Health Organization, in 2010 the death rate from typhus was about one of every 5,000,000 people per year.[21]
Only a few areas of epidemic typhus exist today. Since the late 20th century, cases have been reported in Burundi, Rwanda, Ethiopia, Algeria, and a few areas in South and Central America.[22][23][24][25]
Except for two cases, all instances of epidemic typhus in the United States have occurred east of the Mississippi River. An examination of a cluster of cases in Pennsylvania concluded the source of the infection was flying squirrels.[26] Sylvatic cycle (diseases transmitted from wild animals) epidemic typhus remains uncommon in the US. The Centers for Disease Control and Prevention have documented only 47 cases from 1976 to 2010.[27] An outbreak of flea-borne murine typhus was identified in downtown Los Angeles, California, in October 2018.[28]
History edit
Middle Ages edit
The first reliable description of typhus appears in 1489 AD during the Spanish siege of Baza against the Moors during the War of Granada (1482–1492). These accounts include descriptions of fever; red spots over arms, back, and chest; attention deficit, progressing to delirium; and gangrenous sores and the associated smell of rotting flesh. During the siege, the Spaniards lost 3,000 men to enemy action, but an additional 17,000 died of typhus.[29]
In historical times,[when?] "jail fever" or "gaol fever" was common in English prisons, and is believed by modern authorities to have been typhus. It often occurred when prisoners were crowded together into dark, filthy rooms where lice spread easily. Thus, "imprisonment until the next term of court" was often equivalent to a death sentence. Prisoners brought before the court sometimes infected members of the court.[30] The Black Assize of Exeter 1586 was another notable outbreak. During the Lent assizes court held at Taunton in 1730, gaol fever caused the death of the Lord Chief Baron, as well as the High Sheriff, the sergeant, and hundreds of others. During a time when persons were executed for capital offenses, more prisoners died from 'gaol fever' than were put to death by all the public executioners in the British realm. In 1759, an English authority estimated that each year, a quarter of the prisoners had died from gaol fever.[30] In London, gaol fever frequently broke out among the ill-kept prisoners of Newgate Prison and then moved into the general city population. In May 1750, the Lord Mayor of London, Sir Samuel Pennant, and many court personnel were fatally infected in the courtroom of the Old Bailey, which adjoined Newgate Prison.[31]
Early modern epidemics edit
Epidemics occurred routinely throughout Europe from the 16th to the 19th centuries, including during the English Civil War, the Thirty Years' War, and the Napoleonic Wars.[32] Pestilence of several kinds raged among combatants and civilians in Germany and surrounding lands from 1618 to 1648. According to Joseph Patrick Byrne, "By war's end, typhus may have killed more than 10 percent of the total German population, and disease in general accounted for 90 percent of Europe's casualties."[33]
19th century edit
During Napoleon's retreat from Moscow in 1812, more French soldiers died of typhus than were killed by the Russians.[34]
A major epidemic occurred in Ireland between 1816 and 1819, during the famine caused by a worldwide reduction in temperature known as the Year Without a Summer. An estimated 100,000 people perished. Typhus appeared again in the late 1830s, and yet another major typhus epidemic occurred during the Great Irish Famine between 1846 and 1849. The typhus outbreak along with typhoid fever is said to be responsible for 400,000 deaths.[35] The Irish typhus spread to England, where it was sometimes called "Irish fever" and was noted for its virulence. It killed people of all social classes, as lice were endemic and inescapable, but it hit particularly hard in the lower or "unwashed" social strata.[36]
In the United States, a typhus epidemic broke out in Philadelphia in 1837 and killed the son of Franklin Pierce (14th President of the United States) in Concord, New Hampshire, in 1843. Several epidemics occurred in Baltimore, Memphis, and Washington, DC, between 1865 and 1873. Typhus was also a significant killer during the US Civil War, although typhoid fever was the more prevalent cause of US Civil War "camp fever". Typhoid fever is caused by the bacterium Salmonella enterica Serovar Typhi.[37]
In Canada alone, the typhus epidemic of 1847 killed more than 20,000 people from 1847 to 1848, mainly Irish immigrants in fever sheds and other forms of quarantine, who had contracted the disease aboard the crowded coffin ships in fleeing the Great Irish Famine. Officials neither knew how to provide sufficient sanitation under conditions of the time nor understood how the disease spread.[38]
20th century edit
Typhus was endemic in Poland and several neighboring countries prior to World War I (1914–1918), but became epidemic during the war.[39][40][41] Delousing stations were established for troops on the Western Front during World War I, but typhus ravaged the armies of the Eastern Front, where over 150,000 died in Serbia alone.[42] Fatalities were generally between 10% and 40% of those infected and the disease was a major cause of death for those nursing the sick.[citation needed]
In 1922, the typhus epidemic reached its peak in Soviet territory, with some 20 to 30 million cases in Russia.[43] Although typhus had ravaged Poland with some 4 million cases reported, efforts to stem the spread of disease in that country had largely succeeded by 1921 through the efforts of public health pioneers such as Hélène Sparrow and Rudolf Weigl.[44] In Russia during the civil war between the White and Red Armies, epidemic typhus killed 2–3 million people, many of whom were civilians.[41][43][45][46] In 1937 and 1938 there was a typhus epidemic in Chile.[47]
During World War II, many German POWs after the loss at Stalingrad died of typhus. Typhus epidemics killed those confined to POW camps, ghettos, and Nazi concentration camps who were held in unhygienic conditions. Pictures of mass graves including people who died from typhus can be seen in footage shot at Bergen-Belsen concentration camp.[48] Among thousands of prisoners in concentration camps such as Theresienstadt and Bergen-Belsen who died of typhus[48] were Anne Frank, age 15, and her sister Margot, age 19 in the latter camp.
The first typhus vaccine was developed by the Polish zoologist Rudolf Weigl in the interwar period; the vaccine did not prevent the disease but reduced its mortality.[49]
-
Charles Nicolle received the 1928 Nobel Prize in Medicine for his identification of lice as the transmitter of epidemic typhus.
-
A US soldier is demonstrating DDT hand-spraying equipment. DDT was used to control the spread of typhus-carrying lice.
-
A Civilian Public Service worker distributes rat poison for typhus control in Gulfport, Mississippi, around 1945.
21st century edit
Beginning in 2018, a typhus outbreak spread through Los Angeles County primarily affecting homeless people.[50] In 2019, city attorney Elizabeth Greenwood revealed that she, too, was infected with typhus as a result of a flea bite at her office in Los Angeles City Hall.[51][52] Pasadena also experienced a sudden uptick in typhus with 22 cases in 2018 but, without being able to attribute this to one location, the Pasadena Public Health Department did not identify the cases as an "outbreak".[53] Over the past decade as well murine typhus cases have been rising with the highest number of cases being 171 in 2022.[54]
References edit
- ^ a b c d e f "Typhus Fevers". Centers for Disease Control and Prevention. 7 March 2017. Archived from the original on 26 March 2017. Retrieved 26 March 2017.
- ^ a b c d "Information for Health Care Providers". Centers for Disease Control and Prevention | Typhus Fevers. 7 March 2017. Archived from the original on 27 March 2017. Retrieved 26 March 2017.
- ^ a b c d e f "Epidemic Typhus | Typhus Fevers". Centers for Disease Control and Prevention. 7 March 2017. Archived from the original on 26 March 2017. Retrieved 27 March 2017.
- ^ a b c d "Scrub Typhus". Centers for Disease Control and Prevention. 7 March 2017. Archived from the original on 26 March 2017. Retrieved 26 March 2017.
- ^ a b c d "Murine Typhus". Centers for Disease Control and Prevention. Archived from the original on 26 March 2017. Retrieved 26 March 2017.
- ^ "WHO | Typhus". www.who.int. May 1997. Archived from the original on 27 March 2017. Retrieved 26 March 2017.
- ^ a b Bennett JE, Dolin R, Blaser MJ (2014). Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases E-Book. Elsevier Health Sciences. p. 2217. ISBN 9780323263733. Archived from the original on 2017-09-10.
- ^ Evans AS, Brachman PS (2013). Bacterial Infections of Humans: Epidemiology and Control. Springer. p. 839. ISBN 9781461553274. Archived from the original on 2017-09-10.
- ^ Levinson W (2010). Review of Medical Microbiology and Immunology (11 ed.). McGraw Hill. ISBN 9780071700283.
- ^ Mullen GR, Durden LA (27 September 2002). Medical and Veterinary Entomology. Academic Press. pp. 58–. ISBN 978-0-08-053607-1. Archived from the original on 10 September 2017.
- ^ "Herpes Meningoencephalitis". www.hopkinsmedicine.org. 2019-11-19. Retrieved 2023-10-31.
- ^ Liu X, Zhang Y, Zhang J, Lou Z, Xia H, Lu Z (2021). "The Early Diagnosis of Scrub Typhus by Metagenomic Next-Generation Sequencing". Frontiers in Public Health. 9. doi:10.3389/fpubh.2021.755228. ISSN 2296-2565. PMC 8632043. PMID 34858931.
- ^ Eremeeva ME, Dasch GA (2014). "Rickettsial (Spotted & Typhus Fevers) & Related Infections (Anaplasmosis & Ehrlichiosis)". CDC health Information for International Travel 2014: The Yellow Book. New York. ISBN 978-0-19-994850-5. Archived from the original on 17 May 2014.
{{cite book}}: CS1 maint: location missing publisher (link) - ^ CDC (2021-03-29). "Typhus fevers for healthcare providers | CDC". Centers for Disease Control and Prevention. Retrieved 2023-10-19.
- ^ Chattopadhyay S, Richards AL (2007). "Scrub typhus vaccines: past history and recent developments". Human Vaccines. 3 (3): 73–80. doi:10.4161/hv.3.3.4009. PMID 17375000.
- ^ CDC (2020-11-13). "Scrub typhus | CDC". Centers for Disease Control and Prevention. Retrieved 2023-10-19.
- ^ CDC (2023-08-03). "Flea-borne (murine) typhus | CDC". Centers for Disease Control and Prevention. Retrieved 2023-10-19.
- ^ Heymann D (2015). Control of communicable diseases manual : an official report of the American Public Health Association. Washington, DC: APHA Press, an imprint of the American Public Health Association. pp. 661–668. ISBN 9780875530185.
- ^ "Department of Agriculture | Typhus Fever - Rickettsia prowazekii". www.nj.gov. Retrieved 2023-09-14.
- ^ Matossian RM, Thaddeus J, Garabedian GA (January 1963). "Outbreak of epidemic typhus in the northern region of Saudi Arabia". The American Journal of Tropical Medicine and Hygiene. 12: 82–90. doi:10.4269/ajtmh.1963.12.82. PMID 13933690.
- ^ WHO Statistical Information System (WHOSIS) Archived 2010-02-21 at the Wayback Machine
- ^ Raoult D, Roux V, Ndihokubwayo JB, Bise G, Baudon D, Marte G, Birtles R (1997). "Jail fever (epidemic typhus) outbreak in Burundi". Emerging Infectious Diseases. 3 (3): 357–60. doi:10.3201/eid0303.970313. PMC 2627627. PMID 9284381.
- ^ Mokrani K, Fournier PE, Dalichaouche M, Tebbal S, Aouati A, Raoult D (August 2004). "Reemerging threat of epidemic typhus in Algeria". Journal of Clinical Microbiology. 42 (8): 3898–900. doi:10.1128/jcm.42.8.3898-3900.2004. PMC 497610. PMID 15297561.
- ^ "Epidemic typhus risk in Rwandan refugee camps". Relevé Épidémiologique Hebdomadaire. 69 (34): 259. August 1994. PMID 7947074.
- ^ Perine PL, Chandler BP, Krause DK, McCardle P, Awoke S, Habte-Gabr E, et al. (May 1992). "A clinico-epidemiological study of epidemic typhus in Africa". Clinical Infectious Diseases. 14 (5): 1149–58. doi:10.1093/clinids/14.5.1149. PMID 1600020.
- ^ Chapman AS, Swerdlow DL, Dato VM, Anderson AD, Moodie CE, Marriott C, et al. (July 2009). "Cluster of sylvatic epidemic typhus cases associated with flying squirrels, 2004-2006". Emerging Infectious Diseases. 15 (7): 1005–11. doi:10.3201/eid1507.081305. PMC 2744229. PMID 19624912.
- ^ McQuiston JH, Knights EB, Demartino PJ, Paparello SF, Nicholson WL, Singleton J, et al. (September 2010). "Brill-Zinsser disease in a patient following infection with sylvatic epidemic typhus associated with flying squirrels". Clinical Infectious Diseases. 51 (6): 712–5. doi:10.1086/655891. PMID 20687836.
- ^ "Downtown LA Hit With Outbreak Of Flea-Borne Typhus". CBS Los Angeles. 4 October 2018.
- ^ Zinsser H (1960). Rats, Lice and History. Bantam Classic. p. 186.
- ^ a b Smith RD (January 1967). "Criminal Law—Arrest—The Right to Resist Unlawful Arrest". Natural Resources Journal. 7 (1): 119–28. (hereinafter Comment) (citing Howard J (1929). The State of the Prisons. J.M. Dent & Sons Ltd. pp. 6–7. (Howard's observations are from 1773 to 1775). Copied from State v. Valentine (May 1997) 132 Wn.2d 1, 935 P.2d 1294
- ^ Gordon, Charles The Old Bailey and Newgate Archived 2016-03-12 at the Wayback Machine pp.331–2. T. Fisher Unwin, London, 1902
- ^ War and Pestilence Archived 2009-09-21 at the Wayback Machine. Time magazine
- ^ Byrne JP (2008). Encyclopedia of Pestilence, Pandemics, and Plagues: A—M. ABC-CLIO. p. 732. ISBN 978-0-313-34102-1. Archived from the original on 2014-01-04.
- ^ The Historical Impact of Epidemic Typhus Archived 2009-11-06 at the Wayback Machine. Joseph M. Conlon.
- ^ Ó Gráda C (1999). Black '47 and Beyond: The Great Irish Famine in History, Economy, and Memory. Princeton University Press. p. 88.
- ^ Renvoise A, Raoult D (2013-01-01), Magill AJ, Hill DR, Solomon T, Ryan ET (eds.), "61 - Epidemic Louse-borne Typhus", Hunter's Tropical Medicine and Emerging Infectious Disease (Ninth Edition), London: W.B. Saunders, pp. 535–538, ISBN 978-1-4160-4390-4, retrieved 2023-10-31
- ^ Dougan G, Baker S (2014-09-08). "Salmonella enterica serovar Typhi and the pathogenesis of typhoid fever". Annual Review of Microbiology. 68 (1): 317–36. doi:10.1146/annurev-micro-091313-103739. PMID 25208300.
- ^ "M993X.5.1529.1 | The government inspector's office". McCord Museum. Montreal. Archived from the original on 8 April 2011. Retrieved 22 January 2012.
- ^ "Health, Disease, Mortality; Demographic Effects | International Encyclopedia of the First World War (WW1)". encyclopedia.1914-1918-online.net. Retrieved 2021-02-26.
- ^ Goodall ES (April 23, 1920). "Typhus Fever in Poland, 1916 to 1919". Section of Epidemiology and State Medicine. 13 (Sect Epidemiol State Med): 261–276. PMC 2152684. PMID 19981289.
- ^ a b "Typhus, War, and Vaccines". History of Vaccines. Archived from the original on 2021-02-28. Retrieved 2021-02-26.
- ^ Pennington H (February 2019). "The impact of infectious disease in war time: a look back at WW1". Future Microbiology. 14 (3): 165–168. doi:10.2217/fmb-2018-0323. PMID 30628481.
- ^ a b Patterson KD (October 1993). "Typhus and its control in Russia, 1870-1940". Medical History. 37 (4): 361–81. doi:10.1017/s0025727300058725. PMC 1036775. PMID 8246643.
- ^ Paul Weindling. International Health Organisations and Movements, 1918–1939. Cambridge University Press 1995, p. 99.
- ^ Andrew W. Artenstein. Vaccines: A Biography. Springer 2010, p. 250
- ^ David G. Rempel. A Mennonite Family in Tsarist Russia and the Soviet Union, 1789–1923. University of Toronto Press 2011, p. 249
- ^ Fever in Chile
- ^ a b Trials of War Criminals Before the Nuernberg Military Tribunal (PDF). Vol. 1. U.S. Government Printing Office. 1949. pp. 508–511. Archived (PDF) from the original on 4 March 2016. Retrieved 19 May 2015.
- ^ Naomi Baumslag, Murderous Medicine: Nazi Doctors, Human Experimentation, and Typhus, Greenwood Publishing Group, 2005, page 133 Archived 2014-06-27 at the Wayback Machine
- ^ Grover J, Corral A. "Typhus Epidemic Worsens in Los Angeles". NBC Southern California. Retrieved 9 February 2019.
- ^ Smith D. "L.A. City Hall, overrun with rats, might remove all carpets amid typhus fears". Los Angeles Times.
- ^ City News Service. "Amid Typhus Outbreak, LA City Hall Carpets May Be Ripped Out". NBC Southern California. Retrieved 12 February 2019.
- ^ Braslow S. "How the Homeless Ended Up Being Blamed for Typhus". Los Angeles Magazine. Retrieved 5 March 2021.
- ^ Alarcón J (2023). "Fleaborne Typhus–Associated Deaths — Los Angeles County, California, 2022". MMWR. Morbidity and Mortality Weekly Report. 72 (31): 838–843. doi:10.15585/mmwr.mm7231a1. ISSN 0149-2195. PMC 10414999. PMID 37535465.