Pelizaeus–Merzbacher disease is an X-linked neurological disorder that damages oligodendrocytes in the central nervous system. It is caused by mutations in proteolipid protein 1 (PLP1), a major myelin protein. It is characterized by a decrease in the amount of insulating myelin surrounding the nerves (hypomyelination) and belongs to a group of genetic diseases referred to as leukodystrophies.[2]
| Pelizaeus–Merzbacher disease | |
|---|---|
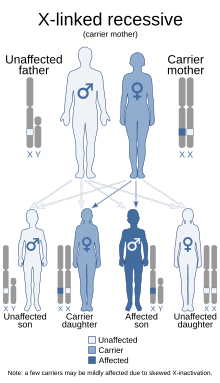 | |
| Pelizaeus–Merzbacher disease is inherited in an x-linked recessive manner[1] | |
| Specialty | Neurology |
Signs and symptoms edit
The hallmark signs and symptoms of Pelizaeus–Merzbacher disease include little or no movement in the arms or legs, respiratory difficulties, and characteristic horizontal movements of the eyes left to right.[citation needed]
The onset of Pelizaeus–Merzbacher disease is usually in early infancy. The most characteristic early signs are nystagmus (rapid, involuntary, rhythmic motion of the eyes) and low muscle tone. Motor abilities are delayed or never acquired, mostly depending upon the severity of the mutation. Most children with Pelizaeus–Merzbacher disease learn to understand language, and usually have some speech. Other signs may include tremor, lack of coordination, involuntary movements, weakness, unsteady gait, and over time, spasticity in legs and arms. Muscle contractures often occur over time. Mental functions may deteriorate. Some patients may have convulsions and skeletal deformation, such as scoliosis, resulting from abnormal muscular stress on bones.[3]
Cause edit
Pelizaeus–Merzbacher disease is caused by X-linked recessive mutations in the major myelin protein proteolipid protein 1 (PLP1). This causes hypomyelination in the central nervous system and severe neurological disease. The majority of mutations result in duplications of the entire PLP1 gene. Deletions of PLP1 locus (which are rare) cause a milder form of Pelizaeus–Merzbacher disease than is observed with the typical duplication mutations, which demonstrates the critical importance of gene dosage at this locus for normal CNS function.[4]
Diagnosis edit
The diagnosis of Pelizaeus–Merzbacher disease is often first suggested after identification by magnetic resonance imaging of abnormal white matter (high T2 signal intensity, i.e. T2 lengthening) throughout the brain, which is typically evident by about 1 year of age, but more subtle abnormalities should be evident during infancy. Unless a family history consistent with sex-linked inheritance exists, the condition is often misdiagnosed as cerebral palsy. Once a PLP1 mutation is identified, prenatal diagnosis or preimplantation genetic diagnostic testing is possible.[citation needed]
Classification edit
The disease is one in a group of genetic disorders collectively known as leukodystrophies that affect the growth of the myelin sheath, the fatty covering—which acts as an insulator—on nerve fibers in the central nervous system. The several forms of Pelizaeus–Merzbacher disease include classic, congenital, transitional, and adult variants.[5] Pelizaeus–Merzbacher disease is the common name for hypomyelinating leukodystrophies (HLD).[6] There are at least 26 HLD variants cataloged by the National Institutes of Health National Library of Medicine[7] and the Online Mendelian Inheritance in Man (OMIM) compendium of human genes and genetic phenotypes.[8]
Milder mutations of the PLP1 gene that mainly cause leg weakness and spasticity, with little or no cerebral involvement, are classified as spastic paraplegia 2 (SPG2).[citation needed]
Treatment edit
No cure for Pelizaeus–Merzbacher disease has been developed.[9] Outcomes are variable: people with the most severe form of the disease do not usually survive to adolescence, although with milder forms, survival into adulthood is possible.[9]
A phase I clinical trial using an antisense oligonucleotide (known as ION356) targeted against PLP1 is expected to begin in early 2024.[10]
Research edit
In December 2008, StemCells, Inc received clearance in the United States to conduct a phase I clinical trials of human neural stem cell transplantation.[11] The trial did not show meaningful efficacy and the company has since gone bankrupt.[12]
In 2019 Paul Tesar, a professor at Case Western Reserve University, used CRISPR and antisense therapy in a mouse model of Pelizaeus–Merzbacher with success.[13][14][15] In 2022 Case Western Reserve University entered an exclusive licensing agreement with Ionis Pharmaceuticals to develop a human treatment for the disorder.[16]
See also edit
References edit
- ^ "OMIM Entry - # 312080 - Pelizaeus-Merzbacher Disease; PMD". omim.org. Retrieved 5 August 2017.
- ^ Hobson, Grace; Garbern, James (2012). "Pelizaeus-Merzbacher Disease, Pelizaeus-Merzbacher-Like Disease 1, and Related Hypomyelinating Disorders". Seminars in Neurology. 32 (1): 062–067. doi:10.1055/s-0032-1306388. ISSN 0271-8235. PMID 22422208. S2CID 25529422.
- ^ "Pelizaeus-Merzbacher disease: MedlinePlus Genetics". medlineplus.gov. Retrieved 2022-06-25.
- ^ Sima, A.A.F.; Pierson, C.R.; Woltjer, R.L.; et, al (2009). "Neuronal loss in Pelizaeus–Merzbacher disease differs in various mutations of the proteolipid protein 1". Acta Neuropathol. 118 (4): 531–539. doi:10.1007/s00401-009-0562-8. PMC 3876935. PMID 19562355. Retrieved January 14, 2024.
- ^ "Pelizaeus-Merzbacher disease (Concept Id: C0205711) - MedGen - NCBI". www.ncbi.nlm.nih.gov. Retrieved 2021-03-03.
- ^ Wolf, Nicole; Ffrench-Constant, Charles; van der Knaap, Marjo (2021). "Hypomyelinating leukodystrophies — unravelling myelin biology". Nat Rev Neurol. 17 (2): 88-103. doi:10.1038/s41582-020-00432-1. PMID 33324001. S2CID 229182946.
- ^ "National Library of Medicine". National Institutes of Health. Retrieved 7 March 2024.
- ^ "Online Mendelian Inheritance in Man". Johns Hopkins University.
- ^ a b "Pelizaeus-Merzbacher Disease Information Page". National Institute of Neurological Disorders and Stroke.
- ^ "Ionis Innovation Day". Retrieved October 4, 2023.
- ^ "Stem Cells, Inc".
- ^ "End of line for StemCells Inc., pioneering & controversial stem cell biotech". 2016-05-31.
- ^ Elitt, Matthew S.; Barbar, Lilianne; Shick, H. Elizabeth; Powers, Berit E.; Maeno-Hikichi, Yuka; Madhavan, Mayur; Allan, Kevin C.; Nawash, Baraa S.; Nevin, Zachary S.; Olsen, Hannah E.; Hitomi, Midori; LePage, David F.; Jiang, Weihong; Conlon, Ronald A.; Rigo, Frank; Tesar, Paul J. (31 December 2018). "Therapeutic suppression of proteolipid protein rescues Pelizaeus-Merzbacher Disease in mice" (PDF). bioRxiv: 508192. doi:10.1101/508192.
- ^ Elitt, Matthew S.; Barbar, Lilianne; Shick, H. Elizabeth; Powers, Berit E.; Maeno-Hikichi, Yuka; Madhavan, Mayur; Allan, Kevin C.; Nawash, Baraa S.; Gevorgyan, Artur S.; Hung, Stevephen; Nevin, Zachary S.; Olsen, Hannah E.; Hitomi, Midori; Schlatzer, Daniela M.; Zhao, Hien T.; Swayze, Adam; Lepage, David F.; Jiang, Weihong; Conlon, Ronald A.; Rigo, Frank; Tesar, Paul J. (2020-07-01). "Suppression of proteolipid protein rescues Pelizaeus-Merzbacher Disease". Nature. 585 (7825): 397–403. Bibcode:2020Natur.585..397E. doi:10.1038/s41586-020-2494-3. PMC 7810164. PMID 32610343.
- ^ "Research finds new approach to treating certain neurological diseases". MedicalXpress. 1 July 2020. Retrieved 1 July 2020.
Their research was published online July 1 in the journal Nature. "The pre-clinical results were profound. PMD mouse models that typically die within a few weeks of birth were able to live a full lifespan after treatment," said Paul Tesar
- ^ "Case Western Reserve University grants exclusive license to Ionis Pharmaceuticals to advance antisense therapy for Pelizaeus-Merzbacher disease". The Daily. 2022-01-27. Retrieved 2022-03-06.
Further reading edit
- Uhlenberg, Birgit; Schuelke, Markus; Rüschendorf, Franz; Ruf, Nico; Kaindl, Angela M.; Henneke, Marco; Thiele, Holger; Stoltenburg-Didinger, Gisela; Aksu, Fuat; Topaloğlu, Haluk; Nürnberg, Peter; Hübner, Christoph; Weschke, Bernhard; Gärtner, Jutta (August 2004). "Mutations in the Gene Encoding Gap Junction Protein α12 (Connexin 46.6) Cause Pelizaeus-Merzbacher–Like Disease". The American Journal of Human Genetics. 75 (2): 251–260. doi:10.1086/422763. PMC 1216059. PMID 15192806.
External links edit
- Pelizaeus-Merzbacher Disease - PMD Foundation
- Pelizaeus-Merzbacher Disease Archived 2008-10-07 at the Wayback Machine. NINDS/National Health Institutes.
- pmd at NIH/UW GeneTests