Nail clubbing, also known as digital clubbing or clubbing, is a deformity of the finger or toe nails associated with a number of diseases, anomalies and defects; some congenital. This is mostly of the heart and lungs.[2][3] When it occurs together with joint effusions, joint pains, and abnormal skin and bone growth it is known as hypertrophic osteoarthropathy.[4]
| Clubbing | |
|---|---|
| Other names | Drumstick fingers/toes, Hippocratic fingers/toes, digital clubbing, watch-glass nails[1] |
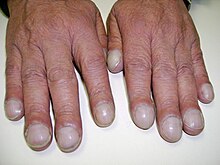 | |
| Clubbing | |
| Specialty | Pulmonology |
Clubbing is associated with lung cancer, lung infections, interstitial lung disease, cystic fibrosis, or cardiovascular disease.[5] Clubbing may also run in families,[5] and occur unassociated with other medical problems.[6][7]
Clubbing has been recognized as a sign of disease since the time of Hippocrates.[5]
Causes
editClubbing is associated with
- Lung disease:
- Lung cancer[8]
- Interstitial lung disease most commonly idiopathic pulmonary fibrosis
- Complicated tuberculosis
- Suppurative lung disease: lung abscess, empyema, bronchiectasis, cystic fibrosis
- Mesothelioma of the pleura
- Arteriovenous fistula or malformation
- Sarcoidosis
- Heart disease:
- Any disease featuring chronic hypoxia
- Congenital cyanotic heart disease (most common cardiac cause)
- Subacute bacterial endocarditis
- Atrial myxoma (benign tumor)
- Tetralogy of Fallot
- Gastrointestinal and hepatobiliary:
- Malabsorption
- Crohn's disease and ulcerative colitis
- Cirrhosis, especially in primary biliary cholangitis[9]
- Hepatopulmonary syndrome, a complication of cirrhosis[10]
- Others:
- Graves' disease (autoimmune hyperthyroidism) – in this case it is known as thyroid acropachy[11]
- Familial and hereditary clubbing and "pseudoclubbing" (people of African descent often have what appears to be clubbing)
- Vascular anomalies of the affected arm such as an axillary artery aneurysm (in unilateral clubbing)
Nail clubbing is not specific to chronic obstructive pulmonary disease (COPD). Therefore, in patients with COPD and significant degrees of clubbing, a search for signs of bronchogenic carcinoma (or other causes of clubbing) might still be indicated.[12] A congenital form has also been recognized.[13]
Hypertrophic pulmonary osteoarthropathy
editA special form of clubbing is hypertrophic pulmonary osteoarthropathy (HPOA), known in continental Europe as Pierre Marie-Bamberger syndrome. This is the combination of clubbing and thickening of periosteum (connective tissue lining of the bones) and synovium (lining of joints), and is often initially diagnosed as arthritis. It is commonly associated with lung cancer.[citation needed]
Primary hypertrophic osteoarthropathy
editPrimary hypertrophic osteoarthropathy is HPOA without signs of pulmonary disease. This form has a hereditary component, although subtle cardiac abnormalities can occasionally be found. It is known eponymously as the Touraine–Solente–Golé syndrome. This condition has been linked to mutations in the gene on the fourth chromosome (4q33-q34) coding for the enzyme 15-hydroxyprostaglandin dehydrogenase (HPGD); this leads to decreased breakdown of prostaglandin E2 and elevated levels of this substance.[14]
Pathogenesis
editThe exact cause for sporadic clubbing is unknown. Theories as to its cause include:
- Vasodilation (i.e., distended blood vessels).[citation needed]
- Secretion of growth factors (e.g., platelet-derived growth factor and hepatocyte growth factor) from the lungs.[citation needed]
- Overproduction of prostaglandin E2 by other tissues.[14]
- Increased entry of megakaryocytes into the systemic circulation. Under normal circumstances in healthy individuals, megakaryocytes that arise from the bone marrow are trapped in the pulmonary capillary bed and broken down before they enter the systemic circulation. It is thought that in disorders where there is right-to-left shunting or lung malignancy, the megakaryocytes can bypass the breakdown within the pulmonary circulation and enter the systemic circulation. They are then trapped within the capillary beds within the extremities, such as the digits, and release platelet-derived growth factor (PDGF) and vascular endothelial growth factor (VEGF). PDGF and VEGF have growth promoting properties and cause connective tissue hypertrophy and capillary permeability.[15]
Diagnosis
editWhen clubbing is observed, pseudoclubbing[further explanation needed] should be excluded before making the diagnosis. Associated conditions may be identified by taking a detailed medical history—particular attention is paid to lung, heart, and gastrointestinal conditions—and conducting a thorough clinical examination, which may disclose associated features relevant to the underlying diagnosis. Additional studies such as a chest X-ray and a chest CT-scan may reveal otherwise asymptomatic cardiopulmonary disease.[12]
Stages
editClubbing is present in one of five stages:[12]
- No visible clubbing - Fluctuation (increased ballotability) and softening of the nail bed only. No visible changes of nails.
- Mild clubbing - Loss of the normal <165° angle (Lovibond angle) between the nailbed and the fold (cuticula). Schamroth's window (see image) is obliterated. Clubbing is not obvious at a glance.
- Moderate clubbing - Increased convexity of the nail fold. Clubbing is apparent at a glance.
- Gross clubbing - Thickening of the whole distal (end part of the) finger (resembling a drumstick)
- Hypertrophic osteoarthropathy - Shiny aspect and striation of the nail and skin
Schamroth's sign or Schamroth's window test (originally demonstrated by South African cardiologist Leo Schamroth on himself)[16] is a popular test for clubbing. When the distal phalanges (bones nearest the fingertips) of corresponding fingers of opposite hands are directly opposed (place fingernails of same finger on opposite hands against each other, nail to nail), a small diamond-shaped "window" is normally apparent between the nailbeds. If this window is obliterated, the test is positive and clubbing is present.
-
Severe clubbing
-
Front view
-
Side views
-
Cyanotic nail beds
Epidemiology
editThe exact frequency of clubbing in the population is not known. A 2008 study found clubbing in 1%, or 15 patients, of 1511 patients admitted to a department of internal medicine in Belgium. Of these, 40%, or 6 patients, turned out to have significant underlying disease of various causes, while 60%, or 9 patients, had no medical problems on further investigations and remained well over the subsequent year.[7]
History
editAt least since the time of Hippocrates, clubbing has been recognized as a sign of disease.[5] The phenomenon has been called "Hippocratic fingers".
The Dutch painter Dick Ket had nail clubbing as is seen from his paintings. He had an underlying disease, probably dextrocardia.[17]
See also
edit- Clubbed thumb (unrelated congenital deformity)
References
edit- ^ Rapini, Ronald P., Bolognia, Jean L., Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 978-1-4160-2999-1.
- ^ Rutherford JD (14 May 2013). "Digital clubbing". Circulation. 127 (19): 1997–9. doi:10.1161/circulationaha.112.000163. PMID 23671180.
- ^ Freedberg, et al. (2003). Fitzpatrick's Dermatology in General Medicine. (6th ed.). McGraw-Hill. ISBN 0-07-138076-0. : 656
- ^ Krugh M, Vaidya PN (January 2019). Osteoarthropathy Hypertrophic. StatPearls Publishing. PMID 31082012.
- ^ a b c d Burcovschii S, Aboeed A (January 2019). Nail Clubbing. StatPearls Publishing. PMID 30969535.
- ^ Schwatz RA. "Clubbing of the Nails". Medscape. Retrieved 14 August 2014.
- ^ a b Vandemergel X, Renneboog B (July 2008). "Prevalence, aetiologies and significance of clubbing in a department of general internal medicine". Eur. J. Intern. Med. 19 (5): 325–9. doi:10.1016/j.ejim.2007.05.015. PMID 18549933.
- ^ Sridhar KS, Lobo CF, Altman RD (1998). "Digital clubbing and lung cancer". Chest. 114 (6): 1535–37. doi:10.1378/chest.114.6.1535. PMID 9872183.
- ^ Epstein O, Dick R, Sherlock S (1981). "Prospective study of periostitis and finger clubbing in primary biliary cirrhosis and other forms of chronic liver disease". Gut. 22 (3): 203–6. doi:10.1136/gut.22.3.203. PMC 1419499. PMID 7227854.
- ^ Naeije R (March 2003). "Hepatopulmonary syndrome and portopulmonary hypertension". Swiss Med Wkly. 133 (11–12): 163–9. doi:10.4414/smw.2003.10016. PMID 12715285.
- ^ "acropachy". GPnotebook.
- ^ a b c Myers KA, Farquhar DR (2001). "The rational clinical examination: does this patient have clubbing?". JAMA. 286 (3): 341–7. doi:10.1001/jama.286.3.341. PMID 11466101.
- ^ Shah K, Ferrara TM, Jan A, Umair M, Irfanullah, Khan S, Ahmad W, Spritz RA (August 2017). "Homozygous SLCO2A1 translation initiation codon mutation in a Pakistani family with recessive isolated congenital nail clubbing". Br. J. Dermatol. 177 (2): 546–548. doi:10.1111/bjd.15094. PMID 27681482. S2CID 28251025.
- ^ a b Uppal S, Diggle CP, Carr IM, et al. (June 2008). "Mutations in 15-hydroxyprostaglandin dehydrogenase cause primary hypertrophic osteoarthropathy". Nat. Genet. 40 (6): 789–93. doi:10.1038/ng.153. PMID 18500342. S2CID 23484059.
- ^ Dickinson CJ, Martin JF (19 December 1987). "Megakaryocytes and platelet clumps as the cause of finger clubbing". Lancet. 2 (8573): 1434–5. doi:10.1016/s0140-6736(87)91132-9. PMID 2891996. S2CID 43847925.
- ^ Schamroth L (February 1976). "Personal experience". S. Afr. Med. J. 50 (9): 297–300. PMID 1265563.
- ^ (in Dutch) Dick Ket, een schilder en zijn ziekte W.H.D. de Haas, Nederlands Tijdschrift voor Geneeskunde, 1984