Ganciclovir, sold under the brand name Cytovene among others, is an antiviral medication used to treat cytomegalovirus (CMV) infections.
 | |
 | |
| Clinical data | |
|---|---|
| Pronunciation | /ɡænˈsaɪkləvɪər/ |
| Trade names | Cytovene; Cymevene; Vitrasert |
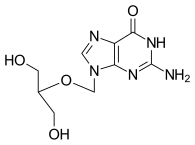
| Other names | gancyclovir; DHPG; 9-(1,3-dihydroxy-2-propoxymethyl)guanine |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a605011 |
| License data |
|
| Pregnancy category |
|
| Routes of administration | Intravenous, by mouth, intravitreal |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | 5% (oral) |
| Metabolism | guanylate kinase (CMV UL97 gene product) |
| Elimination half-life | 2.5–5 hours |
| Excretion | Kidney |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| CompTox Dashboard (EPA) | |
| ECHA InfoCard | 100.155.403 |
| Chemical and physical data | |
| Formula | C9H13N5O4 |
| Molar mass | 255.234 g·mol−1 |
| 3D model (JSmol) | |
| Melting point | 250 °C (482 °F) (dec.) |
| |
| |
| (verify) | |
Ganciclovir was patented in 1980 and approved for medical use in 1988.[3]
Medical use edit
Ganciclovir is indicated for:[4]
- Sight-threatening CMV retinitis in severely immunocompromised people
- CMV pneumonitis in bone marrow transplant recipients
- Prevention of CMV disease in bone marrow and solid organ transplant recipients
- Confirmed CMV retinitis in people with AIDS (intravitreal implant)
It is also used for acute CMV colitis in HIV/AIDS and CMV pneumonitis in immunosuppressed patients.[medical citation needed]
Ganciclovir has also been used with some success in treating Human herpesvirus 6 infections.[5]
Ganciclovir has also been found to be an effective treatment for herpes simplex virus epithelial keratitis.[6]
Veterinary use edit
Ganciclovir (in gel form) appears to be effective for treating the ophthalmic Felid herpesvirus 1 (FHV-1) virus infection in cats.[7]
Adverse effects edit
Ganciclovir is commonly associated with a range of serious haematological adverse effects. Common adverse drug reactions (≥1% of patients) include: granulocytopenia, neutropenia, anaemia, thrombocytopenia, fever, nausea, vomiting, dyspepsia, diarrhea, abdominal pain, flatulence, anorexia, raised liver enzymes, headache, confusion, hallucination, seizures, pain and phlebitis at injection site (due to high pH), sweating, rash, itch, increased serum creatinine and blood urea concentrations.[4]
Toxicity edit
Ganciclovir is considered a potential human carcinogen, teratogen, and mutagen. It is also considered likely to cause inhibition of spermatogenesis. Thus, it is used judiciously and handled as a cytotoxic drug in the clinical setting.[4][8]
Mechanism of action edit
Ganciclovir (9-[(1,3-dihydroxy-2-propoxy)methyl]guanine) is a potent inhibitor of viruses of the herpes family, including cytomegalovirus (CMV), that are pathogenic for humans and animals. The primary mechanism of ganciclovir action against CMV is inhibition of the replication of viral DNA by ganciclovir-5'-triphosphate (ganciclovir-TP). This inhibition includes a selective and potent inhibition of the viral DNA polymerase. Ganciclovir is metabolized to the triphosphate form by primarily three cellular enzymes: (1) a deoxyguanosine kinase induced by CMV-infected cells; (2) guanylate kinase; and (3) phosphoglycerate kinase. Other nucleotide-metabolizing enzymes may be involved as well. The selective antiviral response associated with ganciclovir treatment is achieved because of the much weaker inhibition of cellular DNA polymerases by ganciclovir-TP. Activity and selectivity are also amplified by the accumulation of ganciclovir-TP in CMV-infected cells.
Pharmacokinetics edit
Administration edit
Acute infections are treated in two phases:
- induction phase, 5 mg per kilogram intravenously every 12 hours for 14–21 days, the intravenous dose given as a 1-hour infusion
- maintenance phase, 5 mg per kg intravenously every day
Stable disease is treated with 1000 mg orally three times daily. Similar dosing is used to prevent disease in high-risk patients, such as those infected with human immunodeficiency virus (HIV) or those with organ transplants.
Ganciclovir is also available in slow-release formulations for insertion into the vitreous humour of the eye, as treatment for CMV retinitis (associated with HIV infection).
A topical ophthalmic gel preparation of ganciclovir was recently[when?] approved for the treatment of acute herpes simplex keratitis.[citation needed]
See also edit
Valganciclovir – the prodrug of ganciclovir
References edit
- ^ "FDA-sourced list of all drugs with black box warnings (Use Download Full Results and View Query links.)". nctr-crs.fda.gov. FDA. Retrieved 22 Oct 2023.
- ^ "Prescription medicines: registration of new generic medicines and biosimilar medicines, 2017". Therapeutic Goods Administration (TGA). 21 June 2022. Retrieved 30 March 2024.
- ^ Fischer J, Ganellin CR (2006). Analogue-based Drug Discovery. John Wiley & Sons. p. 504. ISBN 9783527607495.
- ^ a b c Rossi S, ed. (2006). Australian Medicines Handbook. Adelaide: Australian Medicines Handbook. ISBN 0-9757919-2-3.
- ^ Nakano K, Nishinaka K, Tanaka T, Ohshima A, Sugimoto N, Isegawa Y (November 2009). "Detection and identification of U69 gene mutations encoded by ganciclovir-resistant human herpesvirus 6 using denaturing high-performance liquid chromatography". Journal of Virological Methods. 161 (2): 223–230. doi:10.1016/j.jviromet.2009.06.016. PMID 19559728.
- ^ Wilhelmus KR (January 2015). "Antiviral treatment and other therapeutic interventions for herpes simplex virus epithelial keratitis". The Cochrane Database of Systematic Reviews. 1 (1): CD002898. doi:10.1002/14651858.CD002898.pub5. PMC 4443501. PMID 25879115.
- ^ Ledbetter EC, Badanes ZI, Chan RX, Donohue LK, Hayot NL, Harman RM, et al. (June 2022). "Comparative Efficacy of Topical Ophthalmic Ganciclovir and Oral Famciclovir in Cats with Experimental Ocular Feline Herpesvirus-1 Epithelial Infection". Journal of Ocular Pharmacology and Therapeutics. 38 (5): 339–347. doi:10.1089/jop.2022.0001. PMC 9242719. PMID 35613418.
- ^ "Cymevene® (ganciclovir) Australian Approved Product Information". Pharmaco (Australia) Ltd. Australian Therapeutic Goods Administration. 4 November 2022.
Further reading edit
- Noble S, Faulds D (July 1998). "Ganciclovir. An update of its use in the prevention of cytomegalovirus infection and disease in transplant recipients". Drugs. 56 (1): 115–146. doi:10.2165/00003495-199856010-00012. PMID 9664203.
- Spector SA (1999). "Oral Ganciclovir". Antiviral Chemotherapy 5. Advances in Experimental Medicine and Biology. Vol. 458. pp. 121–7. doi:10.1007/978-1-4615-4743-3_11. ISBN 978-1-4613-7150-2. PMID 10549384.
- Couchoud-Heyer C (July 2007). "WITHDRAWN: Cytomegalovirus prophylaxis with antiviral agents for solid organ transplantation". The Cochrane Database of Systematic Reviews (4): CD001320. doi:10.1002/14651858.cd001320.pub2. PMC 10734368. PMID 17636667.