This article needs additional citations for verification. (November 2007) |
In anatomy, the pharyngeal tonsil, also known as the nasopharyngeal tonsil or adenoid, is the superior-most of the tonsils. It is a mass of lymphatic tissue located behind the nasal cavity, in the roof of the nasopharynx, where the nose blends into the throat. In children, it normally forms a soft mound in the roof and back wall of the nasopharynx, just above and behind the uvula.
| Adenoids | |
|---|---|
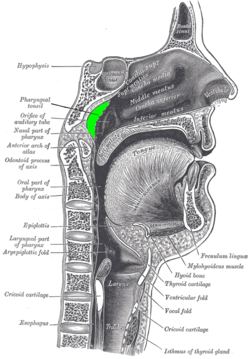 Location of the adenoid | |
| Details | |
| System | Lymphatic system |
| Identifiers | |
| Latin | tonsilla pharyngea |
| MeSH | D000234 |
| TA98 | A05.3.01.006 |
| TA2 | 5186 |
| FMA | 54970 |
| Anatomical terminology | |
The term adenoid is also used to represent adenoid hypertrophy, the abnormal growth of the pharyngeal tonsils.[1]
Structure edit
The adenoid is a mass of lymphatic tissue located behind the nasal cavity, in the roof of the nasopharynx, where the nose blends into the throat. The adenoid, unlike the palatine tonsils, has pseudostratified epithelium.[2] The adenoids are part of the so-called Waldeyer ring of lymphoid tissue which also includes the palatine tonsils, the lingual tonsils and the tubal tonsils.
Development edit
Adenoids develop from a subepithelial infiltration of lymphocytes after the 16th week of embryonic life. After birth, enlargement begins and continues until ages 5 to 7 years.
Function edit
Part of the immune system, adenoids trap and recognize pathogens such as bacteria and viruses. In response, the adenoid produces T cells and B cells to combat infection, contributing to the synthesis of IgA immunoglobulins, assisting in the body's immunologic memory.[3]
Microbiome edit
Species of bacteria such as lactobacilli, anaerobic streptococci, actinomycosis, Fusobacterium species, and Nocardia are normally present by 6 months of age. Normal flora found in the adenoid consists of alpha-hemolytic streptococci and enterococci, Corynebacterium species, coagulase-negative staphylococci, Neisseria species, Haemophilus species, Micrococcus species, and Stomatococcus species.[citation needed]
Clinical significance edit
Enlargement edit
An enlarged adenoid, or adenoid hypertrophy, can become nearly the size of a ping pong ball and completely block airflow through the nasal passages. Even if the enlarged adenoid is not substantial enough to physically block the back of the nose, it can obstruct airflow enough so that breathing through the nose requires an uncomfortable amount of work, and inhalation occurs instead through an open mouth. The enlarged adenoid would also obstruct the nasal airway enough to affect the voice without actually stopping nasal airflow altogether.
Symptomatic enlargement between 18 and 24 months of age is not uncommon, meaning that snoring, nasal airway obstruction and obstructed breathing may occur during sleep. However, this may be reasonably expected to decline when children reach school age, and progressive shrinkage may be expected thereafter.[citation needed]
Adenoid facies edit
Enlargement of the adenoid, especially in children, causes an atypical appearance of the face, often referred to as adenoid facies.[4] Features of adenoid facies include mouth breathing, an elongated face, prominent incisors, hypoplastic maxilla, short upper lip, elevated nostrils, and a high arched palate.[5]
Removal edit
Surgical removal of the adenoid is a procedure called adenoidectomy. Adenoid infection may cause symptoms such as excessive mucus production, which can be treated by its removal. Studies have shown that adenoid regrowth occurs in as many as 19% of the cases after removal.[6] Carried out through the mouth under a general anaesthetic (or less commonly a topical), adenoidectomy involves the adenoid being curetted, cauterized, lasered, or otherwise ablated. The adenoid is often removed along with the palatine tonsils.[7]
See also edit
References edit
- ^ "Definition of ADENOID". www.merriam-webster.com. Retrieved 2018-05-05.
- ^ Histology at KUMC lymphoid-lymph06
- ^ Mnatsakanian, A.; Heil, J. R.; Sharma, S. (2023). "Anatomy, Head and Neck: Adenoids". National Library of Medicine. PMID 30844164. Retrieved 2 June 2023.
- ^ Jefferson, Yosh (2017-02-01). "Mouth breathing: adverse effects on facial growth, health, academics, and behavior". General Dentistry. 58 (1): 18–25, quiz 26–27, 79–80. ISSN 0363-6771. PMID 20129889.
- ^ Wahba, Mohammed. "Adenoid facies". Radiopaedia.org. Radiology Reference Article. Retrieved 2016-11-06.
- ^ Lesinskas, Eugenijus; Drigotas, Martynas (2009-04-01). "The incidence of adenoidal regrowth after adenoidectomy and its effect on persistent nasal symptoms". European Archives of Oto-Rhino-Laryngology. 266 (4): 469–473. doi:10.1007/s00405-008-0892-5. ISSN 1434-4726. PMID 19093130. S2CID 31941117.
- ^ "Adenoids". MedlinePlus, US National Library of Medicine. 13 September 2022. Retrieved 23 July 2023.
External links edit
- "Anatomy diagram: 25420.000-1". Roche Lexicon - illustrated navigator. Elsevier. Archived from the original on 2015-02-26.
- Adenoids: What They Are, How To Recognize Them, What To Do For Them
- Histology at usuhs.mil
- Histology at udel.edu
- /drtbalu otolaryngology online